- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
 I have had a few "higher level" patients in the past few weeks and one consistent trend I found in my practice is that I have been progressing them too quickly. I am not exactly sure why this in the case. Both groups of people present with the same impairments so why would I treat them differently? My assumptions are that I do not want them to become bored with a basic HEP or maybe because they are starting at a higher level they should require higher level exercises. Both of these are fallacies. Despite starting from a higher functional baseline the higher level patients presented with similar impairments as the low level patient. A 3+/5 muscle grade is a 3+/5 no matter how you look at it. For example, with a low level patient, I gave the clamshell exercise to strengthen the posterior gluteus medius. For the higher level, I gave the clamshell exercise in a modified side plank position. Both exercises target similar muscle groups, but the higher level exercise is much more demanding across the entire system. I have given similar exercise prescriptions like this is the past and consistently found that the patient returns to the clinic performing the exercise improperly or having pain while performing it. Lessons Learned: 1. A weak muscle is a weak muscle regardless of what type of patient you find it on. 2. Start basic. In my example above, I added side planks to a clam exercise during the initial HEP. When prescribing this, I made sure the patient had adequate abdominal control, but it took away from the true target of my treatment. The primary impairment was gluteus medius weakness. I needed to start in the least aggressive position and isolate the glut medius. 3. Educate appropriately. My assumption is fairly true in that higher level patients get bored easily with low level exercises. This patient population is used to performing strenuous exercises. Generally, despite being in pain, they want to perform something hard. As a therapist, educating them on the importance of the low level exercises and discussing the exercise progression in future visits will allow for more patient buy-in to your treatment. Do not be afraid to start at the most basic level. You are the expert and you no why they need to start at that level. -Jim
3 Comments
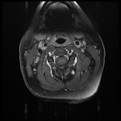 I performed 3 evaluations yesterday morning. The first individual has been having cervical pain since a MVA in 1991, the second low back pain since her first child 7 years ago, and the last individual was having bilateral radicular symptoms for the past 6 months following a discharge from the military. All 3 can be defined as having chronic pain. Knowing their duration of symptoms alone, how does this change my plan of care? How does it change my prognosis? What sort of goals need to be set between the patient and I? When a patient presents to you with pain for >6 months, they often are having pain in multiple joints. This makes sense from both a biomechanical and cortical reorganizing perspective. Biomechanically, if an individual is having pain, they will often start to move more from other body regions to avoid pain. These abnormal movements cause repetitive microstrains and result in pain as well. Additionally, individuals with chronic pain will posture themselves in non-painful positions throughout the day. You will often see them in a guarded, fearful posture. Looking at chronic pain from the cortical level, many changes begin occurring in the cortex in the presence of pain. Cortical smudging occurs and other areas of the brain become activated in the presence of pain. Some of these other areas are those associated with cognitive functioning and emotion so you can imagine how the pain completely envelopes their life. As you can tell already, there is no magical solution to treating these patients. But good approaches include using graded exercises, addressing all barriers that will prevent them from succeeding, and creating realistic and specific goals to measure success. Graded exercise is essential because many of these people STOP exercising in the presence of pain. We see them completely deconditioned, making it difficult to distinguish between true tissue pain or simply the aches and soreness associated with starting a new exercise routine. Start small and start slow! For example, as part of their HEP, I gave one of these patients a home walking program (based off the results of their 6 minute walk test): Walk 4 minutes, 3x/day. Yes, it seems simple, but it is realistic! Barriers also need to be addressed. Typically if someone has been having pain for ~20 years, they have tried to seek care elsewhere but it has been unsuccessful. Why is it unsuccessful? Maybe the musculoskeletal pain is not the only factor. You need to determine if they have financial barriers, transportation issues, psychological issues, social barriers, and more (all of this is obtained during the subjective interview, but gathered much more throughout subsequent visits as you develop a relationship with the patient). Finally, realistic goals must be set. If someone believes they have 10/10 & have been having that pain for 7 years, completely eliminating their pain is not a realistic goal. You need to determine what the patient wants to achieve and set obtainable goals with a set time frame. As you can imagine, adherence and compliance with therapy is another huge problem. Throughout these treatments, education is KEY. Sometimes it may feel that we turn into psychologists. This is partly true, but I say we have a little more power than them. Our research shows that graded exercise is beneficial for individuals with chronic pain. We can spend 1 hour listening to and educating the patient while having them exercise. Early in the treatment you may be taking on a "general exercising and conditioning" approach. This is fine! Stick with it and you will likely find you are often successful. -Jim 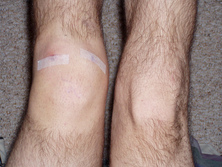 In recent years, Physical Therapy research has emerged that compares surgical interventions to placebo surgeries. For certain conditions, there is now fairly substantial evidence that surgical intervention is not always necessary despite what is considered standard societal practice. The most recent example of this is a December 2013 article written by Sihvonen et al, that investigated arthroscopic surgical menisectomy compared with placebo surgery for individuals with degenerative meniscal tears. The results were pretty interesting! In a recent post by Leonard van Gelder at Dynamic Principles, he discusses the reasons behind why this appears to continually be happening & gives several good examples of when conservative management is either more successful or equally successful as surgery. Questions you need to ask yourself: -If patients have similar results in surgery vs. placebo surgery, what is at fault in the patient? The mechanical system cannot solely be the answer. The answer lies in the patient's belief system regarding tissue healing and surgery. -How should this change the type of education you give a patient regarding certain conditions? -How do you manage a patient that strongly believes surgery is the answer (after a disc herniation for example) despite knowing that surgery is not always the best course of action. (As Leonard discusses in his post, we are well aware that certain conditions require surgical intervention. By no means are we saying surgery is a bad thing. We are simply bringing light to certain conditions that respond positively from conservative management.) |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|







 RSS Feed
RSS Feed