- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
 My cash based Physical Therapy practice, Heafner Health, has been open for 3 weeks now. I have had many questions along the way and already learned some tough lessons. Some of the toughest questions revolve around allocating marketing dollars, professional liability insurance, and documentation. Fortunately, there are plenty of great online resources to help out! In this video call with Aaron LeBauer, we cover a wide variety of topics: -Marketing strategies in the Cash-based setting -How to bill as an out of network provider -Documentation -Online intake forms -Social media advertising Aaron, thank you for the great conversation! Please contact Aaron or myself with questions from the conversation!
-Jim
0 Comments
How do we know when to discharge our patients? Is it when their pain goes away? Is it when they reach their functional goals? Time for discharge is a debatable topic as we should consider risk for re-injury. Unfortunately, there is little evidence that has determined true mobility and strength requirements to prevent risk of re-injury. Looking at current pain science research, imaging has shown many degenerative changes not being correlated with pain. Because of this lack of correlation, should we even be concerned about mobility and strength impairments at discharge? Some recommend we should use joint and muscle "norms" for determining when our patients should be discharged. Personally, I recommend a standardized mobility evaluation like the Selective Functional Movement Assessment (SFMA) as it improves consistency of examination. However, with aging we can expect some loss of mobility in all planes (not as much as is often assumed). This can make sticking to the norms for discharge difficult. What is recommended is to compare a joint's directional loss to the other directions in the same joint and the same direction in the contralateral joint. This can give you a better picture of what is "normal" for that individual patient. Recently, I had an injury that brought this consideration to mind. As many of our followers know, I have posted several self-management cases about myself. What is interesting is that the majority of the injuries have been on the L side and many of them have been linked to dysfunctional sideglides loading the L side. I recently posted a case discussion video on the Insider Access Page about my recent injury. A couple weeks ago I developed L foot pain that I originally figured was metatarsalgia, however, I later believed it was a neuroma (if looking at it pathoanatomically). The pain was located under MTP joints 2-3 on L side and only during push off in gait. After trying to treat it a couple days with more local repeated motions, I switched to treating the spine. This was due to my history of dysfunctional sideglides on that side and also because I noticed the pain was worst after sitting for longer periods. Historically, I have had a loss of ankle DF bilaterally but worse on the L side. This may have been why I developed the symptoms in the L foot. With the loss of ankle DF mobility, more strain is put on the surrounding joints. Even though I am now pain-free, I need to continue treating myself to improve my ankle DF mobility in order to decrease my risk of re-injury. While I should work to make my mobility symmetrical, I should continue to work on improving ankle DF mobility bilaterally for myself as I am dysfunctional according to the SFMA. Check out the Insider Access Page for the full video demonstration and discussion on this self-management case. -Chris
 With March Madness going on, it felt appropriate to touch on the importance of ankle mobility. Basketball players are a prime example of those who tend to lack foot and ankle mobility. However, everyday people need ankle mobility as well. For those of your who prescribe some ankle exercises for your patients, take a look at this article I published a few weeks ago. It has pictures and descriptions for the common person. http://blog.paleohacks.com/ankle-mobility/ - Brian  One of the current health fads involves monitoring activity levels. For example, various watches and phones will monitor how many steps we take each day or remind us to not sit for prolonged periods. While this may be a beneficial starting point, we should be concerned that people will become complacent with a rather low level of activity and exercise. The problem with simply monitoring steps is that it doesn't necessarily encourage you to do anything extra for your health. I can't tell you how many people (not just patients) I talk to that when exercise comes up they say "oh I get my 10,000 steps every day." Many people have that AND MORE in just a normal day walking from place to place. Remember, a normal day in this civilization is still more sedentary than for which the human body is designed. Measuring steps is a nice marker to make sure you do a minimum, but we should encourage more active lifestyles. Another problem with the pedometer-type or general activity measurements is that they typically don't recognize calorie expenditure for other activities. For example, some watches will remind people to get up every hour after sitting still. I have heard of people running a marathon then taking a seat and the watch was reminding them to "get up and exercise!" These same devices may hold walking at a higher value compared to some high intensity-interval training (HIIT), resistance training, stationary cardio, and more. With the benefits of various types of exercise, such as resistance training for bone health and HIIT for cardiovascular health, we should be careful of relying on our smart phones and watches to dictate our exercise and "fitness" levels. While walking can be important for our health, it is essential that we educate our clients on performing various styles of exercise and not relying on walking a minimum number of steps. -Chris Like this post? Check out TSPT Insider Access Page for more exclusive information.
 From my own experiences with knee injuries and my clinical experiences, I do not place much faith in 'special tests' for the knee, especially regarding the meniscus. Following my knee injury, I had clicking and popping, joint line tenderness, pain with flexion and extension overpressure, and a positive McMurray's Test. I had 5/5 predictors for a meniscal tear (I also had a positive Thessaly's test). My MRI showed partial MCL and ACL tears without meniscal involvement. It is my understanding that the popping was occurring from swelling in the joint creating poor joint mechanics. During this experience I did not exhibit any locking or catching, which are two other significant symptoms for referral to Orthopedics. From my past clinical experiences, I would reason that persistent locking and painful catching are two symptoms that warrant orthopedic referral with high potential for surgery.
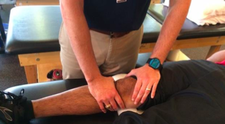 Bottom line: The symptoms don't always match the anatomical tissue involved. Educate your patients that clicking, popping, and locking may be due to swelling, poor NM control, and joint hypomobility. Additionally, educate the importance of high repetition, low resistance exercise to directly target healing of the meniscal tissue. We must treat the impairments present and specifically target the type of tissue involved! I have included both the study from Finland and an article from Regenix. There is obvious bias in the Regenix article so read the literature contained in the article too. Finnish Study Regenix Article -Jim Like this post? Check out TSPT Insider Access Page for more exclusive information.
I recently read an article discussing the need for regular follow-ups for patients following THA to determine the potential need for revisions. As many of you are well aware, with the shift in physical therapy practice shifting towards pain science - based, the question of the necessity comes up regarding joint replacements in the first place. The need for joint replacement is supposed to be based on pain, disability, and loss of joint space. The issue with this is there are plenty of people with loss of joint space that have no pain or disability. It is just a sign of aging on an x-ray. Unfortunately, some in our medical community recommend getting joint replacements if pain ever occurs (even if short-lived) if there is loss of sufficient joint space. I've had patients who have come in for hip or knee pain, for prehab to arthroplasty, that I have eliminated their pain and disability, but they think they still need the surgery! Both practitioners and the patient are at fault. Many clinicians are still stuck in the biomedical model, thinking imaging dictates treatment. Many patients think it is best for them to order medical procedures as if they were on a menu at a restaurant. We must do our best to educate our patients on the potential success for conservative management. Given many patients end up having joint replacements anyway, we must address the question of potential revisions. Revisions typically occur due to infection or pain associated with failure of the prostheses. The article I read mentioned the potential need for long-term follow-up with patients who have had joint replacements and performing imaging to assess the integrity of the prostheses and tissues around them. Currently, patients would only follow-up with an orthopaedic doctor if pain returned to the joint. It is suggested regular follow-up should be performed to assess for potential periprosthetic osteolysis and aseptic loosening. The concern is that these findings contribute to osteolysis and potentially mechanical failure. It is a difficulty decision to make as we often forget the risks associated with any surgical procedure at all (infection, complications from anesthesia, etc.). Even if the patient has pain, with the advancements in pain science, should we let imaging findings dictate our treatment. Honestly, I'm uncertain the best method for managing the potential need for revisions. With normal aging, all developmental processes are associated with biological components. After an arthroplasty, a foreign object is introduced to the body and its malfunction may affect normal processes. Typically the way I manage patients with joint pain with a history of replacement is the same way I treat all my patients: treat the impairments. If I find some muscles are weak, I'm going to try and strengthen them. If I find the lumbar spine is not moving sufficiently, I'm going to try and find a way to improve it. I'll try and reinforce my treatment with education of pain science, as well. However, if a patient fails to respond, I will refer them back to the physician. In summary, I'm not sure it's worth the risk of a revision in asymptomatic patients, due to the potential for infection and the role of the CNS in pain perception. But there likely is still a role for revisions in those with pain, if they fail conservative management. -Chris
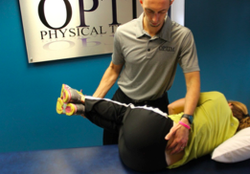
 I've talked about shoulder mobility in some of my past articles but neck stiffness is just as tough. Patients need more and more ways to help treat themselves at home for good compliance. Being able to provide options for patients that are safe and effective is key. Explanations of these exercises is crucial. I recently wrote an article on neck stiffness and a few ways to treat it at home. Feel free to use this article to help with some of your patients. http://blog.paleohacks.com/stiff-neck/ - Brian Physical therapists are good at assessing general lumbar AROM. Our skills often suffer when breaking down the gross active movements into specific segmental mobility testing. When performing lumbar segmental mobility, we should be looking to see if a facet joint is hypomobile. As a general rule, physical therapists are better at assessing hypomobilities than hypermobilities. It is important to assess segmental mobility because this assessment helps the clinician determine which segment is not moving properly. When performing lumbar segmental mobility testing, the examiner should be assessing: 1) Expected normal mobility of the segment 2) Comparing mobility to joints above and below 3) Comparing left to ride asymmetries 4) Consider patient's age, gender, and body type During my lumbar examination, I perform segmental mobility testing after I have watched the patient's functional movements, cardinal plane AROM, PA joint mobility and performed special testing. I am using the findings from each portion of the exam to paint a clinical picture. For example, if the patient is a middle-aged male, acute onset of low back pain, moderate obesity, generally feels "stiff," and lacks adequate cardinal plane AROM, I can confidently assume the patient has some segmental mobility deficits. See below to assess how I perform lumbar segmental mobility. Let me know if you have any questions or comments.
-Jim |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|










 RSS Feed
RSS Feed