- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
Congratulations to all the new physical therapists out there! With the NPTE complete and a horde of new physical therapists searching for the ideal job, one of the most highly sought aspect in a job is mentoring. New grad physical therapists want the opportunity to quickly improve in their new jobs. They want the assistance of those more experienced than them. The problem is most people don't understand what quality mentoring really is. Companies will talk about offering mentoring, but turn around and either never implement it or group it in with occasional journal review or discussion with a colleague. Unfortunately, this may seem like a bonus in many positions due to a history of less than ideal clinical instruction as a student. It's all perspective. Regardless, either the lack of mentoring at all or quality mentoring can lead to the development of poorly designed clinical practice habits. We try A and hope for B. We take a random course that teaches a new tool (dry needling, manipulation, IASTM, etc.) and somehow that develops a pattern of decision making. While we likely see some improved results with these new treatment techniques, we fail to grasp the true understanding of why some patients get better and why some don't. So what is quality mentoring? Those of you familiar with a residency experience likely already have had ideal mentoring. One-on-one with a mentor working on each aspect of case. While that is incredible, it is not exactly necessary. Someone can have a great mentoring experience from a phone call or email if the right components are included. The treatment typically is one of the less important things that should be discussed. The focus should be on the clinical decision making. Why we ask certain questions. Why we assess certain joints and muscles. Why we might choose an exercise or manual technique. It is through these "why's" that we improve our reasoning. Have you ever stopped and asked why you are giving your patient's a certain exercise or doing a certain manual technique? It is easy to fall into the habit of "oh knee pain? I should do some scraping with a tool." Each decision should be supported with a reason. One method of assessing the effectiveness of your intervention is using an asterisk sign. Assess something, treat and reassess. That way you know how successful you were and if you are on the right track. The difficult part is finding these opportunities. Most likely, many of the positions you will interview at will lack the resources for quality mentoring. There are several methods to reach out to potential mentors. One is online or phone. Colleagues can be used for case discussion or philosophy of treatment. There are also clinicians out there who offer some of their time (for a price) specifically for mentoring, like Dr. E at Modern Manual Therapy. Additionally, you can enroll in a program, like a certification series or fellowship that incorporates clinical reasoning development and mentoring. As I said before, a con-ed course where you simply learn a new treatment style does not typically focus on clinical decision making. You want to look for a program that looks to change your practice patterns. One that holds you accountable. Each decision and question should have a reason and it helps to have an experienced clinician guide you there so that you can find your way independently in the future. -Dr. Chris Fox, PT, DPT, OCS
1 Comment
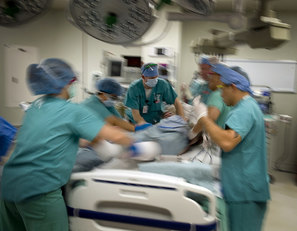 Many in the PT world were excited this past week when the expected systematic review on sham surgeries was released. For the past decade or so, we have come to understand how significant a role the brain plays in the perception of pain and how little the biomechanical aspect actually plays. One of the basis for these pain science developments has been studies looking at placebo treatments and sham surgeries. Many of the recent ones have found that there is no difference between a "real" surgery and a sham surgery. This specific systematic review found sham surgery to be just as beneficial as actual surgery in reducing pain and disability. So what does this mean? First of all, we must be careful before apply these findings to all cases. The systematic review includes a low 6 studies, which is lower than ideal, especially with a total of 277 participants. We also must always remember that, in reality, there is no such thing as a true placebo. We all know a patient's expectations plays a significant role on the outcome of a treatment. If someone expects ultrasound will help them and you completely ignore that expectation, likely that patient will go elsewhere. With these patients, our job is to educate them on the lack of evidence for some treatments and the benefit of others. This part actually supports the findings of the sham surgery systematic review. On the other hand, an incision is not truly a placebo. Following an incision, an inflammatory (healing) response occurs in the region. Maybe the inflammatory process is the most significant factor for some surgeries? We don't know for sure. However, this study can serve as a foundation for further research in pain science and help us to educate our patients on the fact that pathological findings don't necessarily require a surgical intervention. -Chris
 Have you ever seen the extensive list of Clinical Prediction Rule's (CPR's) out there? John Snyder has a good list of them on his website on this page. It is pretty extensive. What most people don't realize is that not all CPR's that we see out there have been validated. A CPR goes through different stages where it is proposed and then proven to be truly applicable. Once it has reached that stage, however, there are many cases where the CPR proves to unuseful. In reality, there is only a certain subset of patients that each CPR applies to, although, it can be extremely effective. I recommend checking out this article by Chad Cook. He explains how a CPR is developed and then some of the pitfalls associated with them as all. It is a perfect example of why we shouldn't handcuff ourselves and our treatment patterns to what is backed by research, and, instead, use it to guide our decision making. This may be an excellent resource for preparing for the NPTE or OCS! -Chris
 The literature over the past several years has demonstrated the direct link between scapular dyskinesias and shoulder dysfunction. For example, if someone lacks Serratus Anterior motor control, it can manifest as the pathoanatomic diagnosis of 'shoulder impingement syndrome.' Good SA strength is essential for normal upward rotation and posterior tipping of the scapula. Clinically when a patient lacks SA motor control, the patient may present with shoulder pain, neck pain, and/or thoracic or rib dysfunction. In this patient scenario, the upper trapezius, scalene muscles, rhomboids, and levator scapulae become dominant and hypertonic. Dominance pattens feed upon themselves until pain or significant dysfunction arises. How the Patient will Compensate for Scapular Weakness Since the scapular stabilizers are not functioning properly, the body develops creative compensations to complete specific movements. First, the patient may demonstrate excessive lower thoracic extension. With increased lower thoracic lordosis, the thoracic paraspinals become dominant. Each time the scapular stabilizers attempt to contract, the thoracic spine locks into extension and powers through the movement using the paraspinals. It will appear that the patient is hinging from the thoracolumbar junction. To retrain this pattern, you need to focus on core position. Have the patient find a neutral spine, then work on retraining the specific scapular dyskinesias. Retraining will often need to happen in a gravity eliminated position (sidelying, prone, or AAROM in supine) because these patients do not know how to activate the scapular stabilizers. A second compensation is excessively using the shoulder external rotators without any scapular stability. This patient will have very dominant Teres Major and Minor muscles and Latissimus Dorsi. A neutral posture for them is retracting the shoulders without any upper thoracic extension. They appear to be in decent postural position, but in reality are lacking proximal/central stability. I often think about this compensation similar to someone who is hamstring dominant. The client appears to have good strength, but they are using prime movers to gain a false sense of stability. In both scenarios, find neutral torso alignment first. This means engaging the deep Transversus Abdominus activation from a long torso position. From here, work on breathing mechanics, ribs mechanics, and engaging deficient muscles. Make sure the patient is not tipping their lower ribs to the pelvis to find a neutral core! Check out the video below which demonstrates the 2 common postural compensations. -Jim Heafner PT, DPT, OCS OPTIM COMT Instructor At Optim Manual Therapy, our goal is not to simply teach a few manipulations or cool new exercises. We want to change your dynamic as a therapist. Again, many programs may talk about incorporating recent evidence, but what's more important is determining the validity of the study and its applicability to our practice. When evaluating a patient, we must consider the individual's biopsychosocial factors, correlation between presentation and anatomical findings, pain science, and evidence-based practice. Our goal is to alter your practice pattern with each patient. Optim Manual Therapy offers a 1-year COMT program in Houston TX, Dallas TX, and Scottsdale AZ. It includes 6 weekend-long onsite classes with lecture and lab, Medbridge classes, online mentoring between classes, and article discussion. Following completion of either a residency or the COMT year, you are welcome to enroll in the Fellowship component. The Fellowship program takes place over 15 months and includes 10 weekend-long courses and 400+ hours of mentoring with a Fellow of the American Academy of Orthopaedic Manual therapy in order to further enhance your clinical reasoning and manual skill development. If you are interested in joining the Optim experience, feel free to contact myself or any of the faculty members. The upcoming Houston TX COMT cohort is already full, but there are still some openings remaining in the Dallas TX and Scottsdale AZ cohorts. Be sure to hurry if interested as classes start in September. Check out www.optimfellowship.com for more information and for some sample material, check out the videos below. -Chris Lecture: Movement Impairment Syndromes and Application to the Lumbar Spine Lecture: Repeated Motions in the Cervicothoracic Spine Online Mentoring Session If you have not had the opportunity to check out PT Pintcast, I highly recommend it. The Pintcast has interviewed many, many excellent Physical Therapists, including the most recent episode with Dr. Dana Tew PT, DPT, OCS, FAAOMPT.
Brief overview of the episode: "In this episode, Jimmy interviews residency and fellowship expert Dana Tew. Dana sips on his go-to Budweiser Select before switching over to his Texan brewed Real Ale Hans’ Pils, while Jimmy taste tests the Green Flash Tangerine Soul Style IPA. Jimmy and Dana discuss the current state of physical therapy residencies and fellowship as well as the future growth of these programs. Creating his own fellowship, Dana keys in on the importance of mentorship in the physical therapy profession and the roles both parties play in fostering a positive learning environment." Interested in doing a residency, fellowship, or advanced education program? Download this episode! One of the components of my residency education at Honor Health and a component that we teach in Optim Manual Therapy COMT/Fellowship programs is Sahrmann's Movement Impairment Syndromes (MIS). For those of you unfamiliar with the topic, MIS involves assessing a painful region for a consistent regular abnormal movement pattern. The theory is established on the premise that normal movement requires a starting point of neutral posture. Should abnormal posture or abnormal repetitive motions be imposed, degenerative conditions may develop in a joint secondary to Wolff's Law. The last part here is definitely debatable with what we now know about pain science. Another potential issue with MIS usage is the case of Double Crush Syndrome or radicular symptoms. While some may think a painful MIS will easily be picked up in the cervical spine upon examination, we must remember that there are cases of Double Crush Syndrome and cervical radiculopathy where no cervical pain is present. The same applies for other regions. Now a therapist using MIS in their assessment and treatment likely would do a thorough evaluation up the chain in order to spot these contributing MIS, but we must remember pain should not necessarily dictate our treatment. Even though the use of MIS may have difficulty with certain diagnoses and the fact that there is a lack of correlation between degenerative conditions and pain, I believe using MIS can be incredibly useful in managing many conditions. While I don't typically treat via a pathoanatomical approach, I do believe that abnormal movement patterns can contribute to the development of pain. For example, an individual who displays lumbar rotation with extension, may show a hypersensitivity to loading the involved side. This pain may be a result of the abnormal movement pattern. This can be addressed with repeated motions, manual therapy, corrective exercises and more. Regardless, ensuring proper movement can decrease the likelihood of reinjur. -Chris
|
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|











 RSS Feed
RSS Feed