- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
 As we have said before, it is not often you see us utilizing a modality due to the lack of evidence. However, there are indeed certain situations with specific pathologies that warrant modality usage. John Snyder at orthopedicmanualpt.com recently did a literature review on the use of NMES for strengthening, especially following surgery. In the article, Snyder reviews the research behind weakness following surgery and studies performed showing strength gains with NMES + exercise. While NMES may play a role in your plan of care, we should be certain to include sufficient exercise as NMES alone is not as effective. For more information, check out the article!
2 Comments
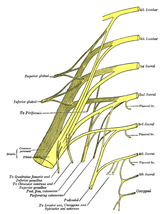 Credit goes to Julie Wiebe for posting this interesting abstract. Overactive Bladder Syndrome (OAB) is a disorder of urgency, frequency, nocturia, and possibly incontinence. This post stood out to us, because the study demonstrated the potential for treating OAB by stimulating the posterior tibial nerve. By inhibiting somatic lumbar and sacral nerve fibers, the detrusor muscle is inhibited without any alteration in the micturition reflex. The study found both ES to the pelvic floor and PTNS to be effective in modulating the effects of OAB; however, ES was found to be superior overall. Yet, it is still interesting to see the effects we can have on the renal system by working peripherally with e-stim. This is something we should consider when treating our patients, for both the potential positive and negative side effects.  As some of you may have noticed, we have a strong interest in evidence-based practice. In fact, one of the missions of this website is to increase awareness of the latest literature. However, to what point should we rely on evidence? Having read more than a few studies that showed little support for modalities in general (Yes, there are some pathologies that respond extremely well), you can imagine we would be hesitant to administer things like ultrasound, hot packs, etc. in the clinic. Coming across patients who request these modalities during treatment can be frustrating as we know they often have little effect physiologically. We have all had the experience of a patient saying, "last time I had therapy, the TENS Machine was really what got me through the day." On one hand you know you do not want to spend valuable treatment time performing these interventions, but on the other you feel it may benefit the patient psychologically. So, where do we go from here? Having recently listened to David Butler's and others' audio recordings from IFOMPT, the importance of the biopsychosocial role really stood out to us. We cannot underestimate the impact of the mind. The neuroplastic changes associated with chronic pain often are as big a part of a patient's complaints as a mechanical component. Patients have been suffering with pain or have had dysfunctional movement for so long that the nervous system has adapted to the new "norm," and it is the true normal movement that feels abnormal. Butler, in fact, states that the biggest predictor of low back pain is depression and that we must explain to patients that the source of there pain is not necessarily mechanical (if a patient is grouped here). So how does this tie in with evidence-based practice? Knowing how the nervous system can affect the patient's perception of pain, there may indeed be a role for interventions with low evidence, such as certain modalities, if a patient believes the treatment will help them return to function. We are not saying that these interventions should consume a significant portion of our treatment time (or that we should go to them at all), but it is something to consider for a trial to calm the patient's fears and give us time for them to "buy into" our methodology, especially if they made a request for that treatment. That being said, we cannot stress enough the importance of educating our patients. Perhaps spend some time explaining to the patient how physiologically, there is little evidence of changes occurring at the cellular level with that specific intervention and then continue to educate the patient on what the literature shows as having the best outcomes. Obviously, education on proper movement patterns and posture must be included as well. You might be surprised at how literal some of our comments are taken. Consider the idea that you teach your patient to lift with a slight lordotic posture, so as to minimalize the stress on the back. Some patients might incorporate this posture into all aspects of their life, thinking that they should never bend their back if they want to avoid pain. Think of all the compensations that might result! We must evaluate all faulty movement patterns a patient presents with and educate them clearly on better strategies. Of course, we should still utilize our clusters, clinical prediction rules, and clinical practice guidelines when treating patients, but we must be aware that not everyone falls into those groupings. Some people have a larger biopsychosocial role than others, and it is these patients that we must spend even more time on education. Yes, maybe we should consider the use of interventions with lower quality evidence early in our treatment plans, but in it, we must include education and interventions with higher quality evidence as well so that we can move toward the desired outcomes.  With the NPTE just a couple weeks away for some of us, we can use as many resources as we can get our hands on! Jordan from Shenandoah University developed this website with a focus on modalities. It breaks down the theory, procedure, and treatment plans for each modality. She even has worksheets included to develop your skills for each modality. There is a lot of useful information here on the subject if you take the time to explore. Thanks for the resource Jordan and good luck to everyone studying for the NPTE!  Stress fractures account for approximately 10% of all athletic injuries. Due to the high amount of impact force, 80-90% of all stress fractures occur in the lower extremities, most commonly seen in the running population. Knowing the high prevalence of stress fractures, it is important to also understand the diagnostic accuracy of the clinical tests one uses to rule-in or rule-less likely a stress fracture. This research article, The Ability of Clinical Tests to Diagnose Stress Fractures: A systematic Review and Meta-analysis, assesses the reliability of both therapeutic ultrasound and the tuning fork test. The review discusses when, why, and how these tests should be implemented. As Schneiders et al, points out "clinically lower-limb stress fractures can be difficult to diagnose, due to a wide range of potential differential diagnoses." This differential diagnosis process should include (but not be limited to) compartment syndrome, muscular strain, tendinitis, tendinosis, infection, and nerve entrapment. Additionally, it is important to know the gold standard for ruling in stress fractures. Currently, a triple phase technium-99 bone scan (scintigraphy) is the most accurate method of diagnosing stress fractures with a sensitivity of 100% and specificity of 76%. MRI has also shown to be highly reliable, but due to its expensive cost, they are less frequently used. Additionally, the single photon-emission CT scan is receiving a lot of attention for it's accuracy in diagnosing stress fractures, but further research is needed. As therapists (excluding the military), we do not have the power to order the gold standard tests mentioned above, so we must rely on our own diagnostic tests to help us interpret our patient's clinical presentation. Clinical tests that are currently used and accepted include therapeutic US, the tuning fork test, superficial palpation, and palpable thickening or swelling of periosteum. This review looked at therapeutic US and the tuning fork.
Unfortunately this systematic review concluded that neither test should be used as stand alone measures for diagnosing stress fractures. Therapeutic US pooled sensitivity (64%) and specificity (63%) revealed a low to moderate performance of the test. A meta-analysis was unable to be performed on the tuning fork test. However, one article by Lesho reported high sensitivity (75%) an moderate specificity (67%) when using the 128 Hz tuning fork. Limitations to this study include an inability to perform heterogenity on the articles and a limitation in the time frame of articles reviewed. Reference:
Scneiders A, et al. (2012). The ability of clinical tests to diagnose stress fractures: a systematic review and meta-analysis. JOSPT. 2012; 42.9: 760-771. Web. 1 May 2013.
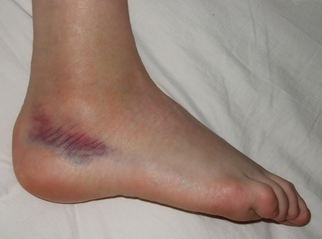
Kelly Starrett from Mobility Wod brought this issue to the light with a post last year. His findings showed that, yes, cryotherapy can be effective in reducing pain following injury, but it was inconclusive as to whether or not it improved clinical outcomes. Again, this modality can be useful in preventing the body from healing its natural way, but do we really want to do that? You might ask then about other methods of limiting pain and swelling in the area. Starrett suggests utilization of compression to limit the swelling, along with elevation at times. Another method to decrease swelling is muscle activation. Mobility (when safe) is an incredibly useful method to a) maintain strength, b) evacuate swelling through muscle pumping, and c) help to restore collagen alignment. Now we're not suggesting ice should suddenly be abandoned in physical therapy altogether, but it should be given a more serious consideration as to its appropriateness. In fact, an interesting response by Nick Heudecker was brought up to this post, questioning the analysis of the literature cited and the method of the studies as well.
Perhaps it is time to consider a shift from the traditional RICE theory to a MEAT theory, as discussed by The Sports Physiotherapist. We have actually seen the MEAT protocol in practice with impressive effectiveness for returning injured athletes to play. M=movement, E=exercise, A=analgesics (non-NSAID), T=treatment. What are your thoughts on the RICE vs MEAT debate? Should we choose one or the other? Or is there a middle-ground that is more desirable? |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|






 RSS Feed
RSS Feed