- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
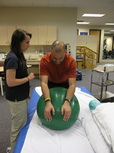 This editorial was brought to me during my residency at Harris Health. It is written by Jason Silvernail on the website SomaSimple. As therapists we often deal with 2 types of pain: Chemical and Mechanical. Understanding the difference between the two is important because it allows you to explain to your patients "why" they are experiencing pain. Chemical Pain is associated with inflammation, and responds positively to anti-inflammatory medication and rest. Mechanical Pain is more complex! It is due to prolonged pressure or tension on nervous tissue. When you see a patient with mechanical pain, they may have questions regarding why their MRI did not show anything significant OR why their medications are not working. This is because Mechanical Pain is due to how the tissue feels, and not the way the tissue looks. There is no acute inflammation and no acute tissue damage. Mechanical pain is a chronic irritation. To fix mechanical pain, we need prescribe movements that relieve the tension that is being placed on the nervous system. This specific movement will gradually or immediately allow the patient to experience less pain. The patient needs to be regularly reversing the postures that are placing tension on their nervous system. This is where doing your Home Exercise Program regularly becomes so important. Sometimes it can be difficult to tell a patient to MOVE when they are in pain, but by educating them that the specific exercises you are prescribing are actually taking tension off the involved structures can be a great for compliance. The last point I will touch on is how many sets and reps should be prescribed for mechanical pain. As therapists, we know how many repetitions to prescribe for strength training, neuromuscular re-education, and power, but how many reps do you prescribe for pain? The answer is unique to each patient and will vary based on comorbidities, irritability level, etc... I would recommend starting with a high repetition, low load dosage. This will minimize the risk for compensations, decrease the risk of increasing symptoms, and hopefully get the patient performing them more frequently. Reference:
Silvernail, J. "Understanding Mechanical Pain." Somasimple.com. Web. 14 Dec. 2013.
2 Comments
 As the year comes to a close I've spent more and more time thinking about how incredible this year has been. Graduating from Saint Louis University's Doctor of Physical Therapy program is at the top of that list. As I have begun my professional career as a physical therapist and sport's resident I have really valued my education that helped me get here. It was that education and relentless commitment from SLU's faculty that game me the tools and necessary skills to build from. After all, we are all adult learners in graduate school. You get what you put in. It was professors like Dr. Ann Hayes who would sit with me and go over orthopedic exam concepts I'd missed or needed more information on. Or professors like Dr. Chris Sebelski who would meet to go over extra movement analysis cases unrelated to any classes for hours. Or Dr. Mark Reinking who would listen and give guidance to any one of the hundreds of nagging sports residency questions I had for him. Or Dr. Darina Sargent who would take the time to stop me in the hallway to tell me about the good things I did in class and give me positive encouragement about my future. The list goes on and on. The point is without my education at Saint Louis University and the amazing faculty who took the time to help me, I would never have had the foundation to start my career the way I have. While the education I am receiving in the residency is incredible, I still find myself going back to some of my notes from PT school to assist my studying. I think it's important to always make sure a physical therapist's foundation is solid. Going back to my SLU notes has helped me keep and build off of my foundation. For students who are looking to attend PT school in the future, I hope Saint Louis University will be in your considerations. More importantly, find a PT school that will go above and beyond for their students like SLU so that you can get as much out of the experience as you put in. - Brian  Our roles as physical therapists is constantly changing & seems to differ extraordinarily depending on what type of patient population you see. Currently, I see A LOT of chronic pain. If someone presents with chronic pain, usually this means the traditional medical model of care will not suffice. In these situations, it is important to use the biopsychosocial model of care if I plan to be successful. Part of the biopsychosocial model is understanding what barriers a person has to therapy. By addressing these barriers, the therapist will best be able to address impairments in the scope of the patient's life. Also by looking at these barriers, you will be able to see if a patient is ready for physical therapy. "Ready" you may be asking yourself? One reality I quickly stumbled across while practicing at a community hospital is that certain people have so many life stresses that take priority before their musculoskeletal health. If a patient comes to see you with cLBP, but also has a history of depression, transportation issues, financial problems, family problems, and reports little to no exercise, strengthening the PGM may not be the first thing they need. I would recommend starting this patient on a general exercise program and a few basic exercises. Going back to barriers, one of the biggest barriers I face each day is patient adherence and compliance. I often struggle with how to address these issues. Which clients are appropriate for PT and which are unfortunately not ready to change? Check out this post by Chris Johnson. He poses some great questions that will put you and the patient on the same level regarding your goals and their expectations of physical therapy. They may save you some time down the road. -Jim  In a recent post, we discussed our experience learning the Selective Functional Movement Assessment (SFMA). A large component of the SFMA is utilizing Rolling Patterns. These patterns are used whenever mobility is cleared and the patient has a pure stability or motor control dysfunction (SMCD). As Gray Cook states in Movement, "Rolling patterns offer a low-load opportunity to review symmetry and motor control, and are even less taxing than quadruped movements." Since the movement is so basic, strength is not what you are assessing. With rolling, the focus is directed toward sequencing, timing, breathing, upper extremity vs. lower extremity disassociation, and of course motor control. Gray also states, "Rolling and quadruped movement patterns are unique observations of fundamental reflex stabilization." In the developmental sequence, rolling is one of the most basic motor patterns. The SFMA assesses 8 different rolling patterns which are a combination of Left vs. Right, Supine vs. Prone, and Upper Extremity vs. Lower Extremity Patterning. On our Multisegmental flexion post, we were asked a question regarding the difference between SFMA rolling and the PNF rolling patterns. From our understanding, the rationale behind both rolling assessments/interventions is the same. Both try to assess side to side symmetry and upper quarter vs. lower quarter symmetry. They both focus on the demands of timing and reflex stabilization. The difference (and not necessarily a difference, but rather treatment style) is how PNF elaborates further on ways to facilitate the incorrect pattern. Someone can definitely utilize different PNF facilitation and inhibition strategies to address rolling in the SFMA, but always allow the patient to self-select a method first before giving any external cues. Without the ability to perform this basic movement properly, how can a patient expect to perform higher level movements? 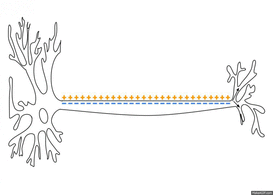 As we have said before, it is not often you see us utilizing a modality due to the lack of evidence. However, there are indeed certain situations with specific pathologies that warrant modality usage. John Snyder at orthopedicmanualpt.com recently did a literature review on the use of NMES for strengthening, especially following surgery. In the article, Snyder reviews the research behind weakness following surgery and studies performed showing strength gains with NMES + exercise. While NMES may play a role in your plan of care, we should be certain to include sufficient exercise as NMES alone is not as effective. For more information, check out the article! Labeling a condition is most often the first step in treatment. Referral sources should expect a label from us. Yet, currently, "Physicians refer to consultants for diagnosis. They refer to PTs for treatment. Autonomy will be actualized when physicians refer to PTs to obtain diagnoses."
|
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|






 RSS Feed
RSS Feed