- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
When doing an examination, one of the goals is to determine the source of the pain or mobility restriction, even though it is not the most important issue. My professional development courses come from a variety of sources and, thus, have different beliefs. Your more traditional manipulative courses believe the origin of all issues comes from the joint. Your myofascial type courses believe the origin is muscular. Typically, we see theses two things occur simultaneously. If you take a look at the spine, for example, you will often see "tender points" at the same level as a hypomobile joint. Which is causing which? If you treat either, usually the other will improve as well.
Personally, I think it is advantageous to include the muscular and joint-based assessment and treatment techniques. Having recently taken a dry needling course, I am recognizing muscle referral patterns I would have previously quickly ran to the spine for diagnosis. While there is likely a link between the two, it may be beneficial to know both the muscular and joint-based involvement. A true muscular referral or radicular referral pattern likely will respond better when the true pain source is treated (as well as the cause). -Chris
0 Comments
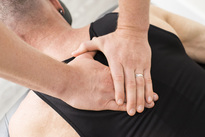 Have you ever stopped to think about how your patient perceives their low back pain? Do patients believe back pain is a normal aspect of aging? Do patients believe surgery is the solution to solving acute mechanical low back pain? As physical therapists, low back pain is by far the most common impairment we treat. Roughly four out of five individuals will experience low back pain at some point during their lives. In previous posts on The Student Physical Therapist, we go into great detail discussing examination and treatment of low back pain. This post has a different focus: our patient's (often flawed) perception of their low back pain. There are so many misconceptions surrounding low back pain. Check out this link from Heafner Health to learn more about the Common Misconceptions regarding Low Back Pain. Misconceptions covered: 1)Misconception 1: The best treatment for low back pain is rest 2)Misconception 2: Back pain is pathological 3) Misconception 3: Back pain means the back is weak 4) Misconception 4: Back pain is a normal part of aging 5) Misconception 5: Disc herniations are the cause of my pain By understanding the common misconceptions, you can better educate your patients regarding their symptoms and prognosis. Since I have been a PT, I have implemented Instrument Assisted Soft Tissue Mobilization (IASTM) into my treatment. Originally, I was trained to "dig deeper" like some of the more prominent brands preach, but advances in research have shown our effects to primarily be neurological and more successful with lighter implementation. Sometimes, no matter how light you perform IASTM in certain areas, you will note some redness developing. These are typically highly tonic areas. Normally, that response may be contraindicated to continue IASTM, but there are ways to adjust. Dr. E from The Manual Therapist recently had a post discussing why these areas can be so easily reddened. He also offers several examples of how to address these instances. Personally, I think these are great tools to implement as I regularly find HS insertions that are significantly tonic and these patients may benefit from these attempts at calming the nervous system. However, I do disagree on "always light" IASTM technique being better. From my experience, I have had a significant number of patients that had previous experiences of different forms of IASTM that are more aggressive with the old school approach. Having tried the lighter technique on these patients, typically they subjectively feel like they don't improve without the more aggressive approach, even if objective results show differently. With what we know about how a patient's beliefs impact their rehabilitation, I tend to be a little more aggressive with my IASTM technique on these patients, although, still not nearly as aggressive as others. -Chris
It is hard to believe I have already been a practicing clinician for 3 years. I know those of you who have been in the clinic for five to ten+ years are laughing right now. Time is not slowing down, which is both exciting and intimidating. Personally, I have found one of the best ways to help slow down is by stopping to reflect on what I have achieved and what I want the future to hold. In this post, I will reflect on what I have learned as a Doctor of Physical Therapy and where our profession needs to go in the years ahead. One of the most foundational concepts I have learned is too keep the treatment sessions simple. We have access to so many resources and new innovative theories, there is a tendency to overcomplicate what we do. When it comes down to it, we are movement specialists. If something is stiff, move it. If something is weak, stabilize it. When a patient scenario is not adding up, there is likely some biopsychosocial variables that need to be addressed. In the end, we need to focus on treating the impairments, and not dwell on the pathoanatomy. Secondly, pain science is the hot topic right now...and rightfully so. If we are not addressing the biopsychosocial aspects of our patients' pain, we are doing them a disservice. Addressing these components is uncomfortable and complicated, but these issues are not going away. As our society continues to grow more obese, over stimulated, and over medicated, the biological and psychological influences of pain will continue to magnify. Physical therapists are one of the only providers to address these components. Combining pain science, manual therapy, and retraining movement patterns will continue to give the best outcomes. 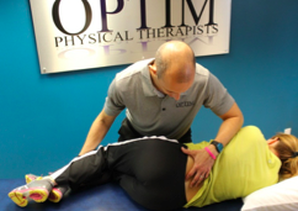 Finally, it is essential to get involved in post-doctoral education. When I graduated from PT school, I knew a little about a wide variety of topics. PTs graduate as a 'jack of all trades, but master of none.' Pursuing a residency program and teaching for OPTIM Manual Therapy Fellowship have allowed my practice to expand in ways I never anticipated. The material that is covered is essential, but even more importantly, the conversations that occur when I surround myself with like minded individuals allows for the greatest growth to occur. As a profession, if we want to continue our path towards direct access and autonomy, it is essential become experts in the field. -Jim Heafner PT, DPT, OCS  Jim earned his Doctorate of Physical Therapy from Saint Louis University. He is a certified Orthopedic Clinical Specialist and trained in the Selective Functional Movement Assessment (SFMA) and Functional Movement Screening (FMS) systems. His educational and clinical background have made him an expert in manual and manipulative physical therapy as well as functional movement. When Jim is not treating patients in the clinic, he focuses his attention on educating fellow physical therapists in the profession, teaching manual therapy courses in Arizona. In addition, his physical therapy based blog attracts upwards of 65,000 views per week. Learn more about Jim by checking out his LinkedIn profile This past weekend, I completed Level 1 Functional Dry Needling certification through Kinetacore. Dry needling had been a tool I wanted to learn for awhile but had been hesitant taking a course due to some states' reluctance to permit PT's to utilize the skill (AZ just accomplished this within the last couple years). However, in looking at the different states' standings, fewer and fewer states restrict dry needling, and most of these states will likely adapt within a few years it would seem. Now, I am not going to write an article discussing the evidence behind dry needling. That is for another time as I already know some people regularly wait to debate the topic. I simply want to review the course. One of the aspects I was most impressed with in the course was the emphasis on examination and test-treat-retest. The instructors did a phenomenal job educating the class on how to properly assess myotomes, incorporate part of the SFMA (Selective Functional Movement Assessment), and, most importantly, how to differentiate between peripheral nerve lesions, radicular lesions, and multi-level involvement. While some of these examination methods are taught in school, many do not fully understand these findings and how it will impact their treatment. With each needling treatment, an asterisk sign was sought and retested afterwards in order to determine the effect of our treatment. Again, this is another component of physical therapy that is regularly missed (often due to time restrictions), but is essential for patient progression. As far as other content goes, the instructors do a good job differentiating between the different theories of how dry needling works and the evidence behind each theory. As with many of our treatments (especially manual), there are different theories out there with evidence to support them, some more than others. This is important as it may impact our treatment. For example, one of the major mechanisms theorized for manipulations and dry needling is through the nervous system. Due to this involvement, almost always related spinal segments are assessed/treated as well. Double Crush Syndrome is a more specific example of this application, but it can also be related to a "strained" hamstring benefiting from treatment to the L5-S1 segments. Additionally, the course covers important topics like the states' rights issue and acupuncture vs. dry needling. One of the major concerns with physical therapists performing dry needling is safety. The concern of infection and transmission is an important one as we are dealing with many patients each day. Clean needle technique is practiced and tested thoroughly to ensure we decrease the risk of these concerns. Other issues like pneumothorax, puncturing arteries, and more are thoroughly covered. In the level 1 course, all techniques are specifically taught to decrease risk of hitting these structures and practiced repeatedly to ensure safety and competence. For example, if treating a muscle that is close to the lungs, it is pulled away from the rib cage and the needle is inserted parallel to the rib cage to avoid any risk of puncturing the lungs. The rib cage itself (and thoracic spine) is completely avoided altogether. Should you follow the instructions from level 1, any risk of severe complication should be significantly reduced. Of course, the most important component is the needling instruction itself. The instructor to student ratio was perfect at 1:6. Each muscle was first reviewed anatomically and the needling technique was discussed afterwards each with pictures and video (3d imaging for muscles/anatomical structures). After that, the large class was broken up into small groups where the instructor reviewed surface anatomy and palpation of landmarks to identify where to treat. The instructors would then demonstrate each needling method and some of their own insight to common findings and tips for treatment. Finally, the small groups were broken up to simply needling your lab partner and then switching, all while the instructors were walking around answering questions and helping the students. I cannot think of one instance where I had to wait more than a minute to have my question answered or to have an instructor assist me. This was done over and over again throughout the weekend to ensure competency with the primary goal of the instructors being to help us safely and competently apply the techniques the next week. Overall, I highly recommend the dry needling course through Kinetacore, even with the cost. The course is organized well to keep your mind attentive and wanting more throughout the weekend. The fact that the material is presented in such an eclectic thought process is pretty impressive for a level 1 course in general. You will come away from the weekend, not only with the ability to safely dry needle right away, but also as a better diagnostician and clinician. Finally, I want to add that each and every instructor emphasized that they would never want any of the students to become "dry needlers," but instead to add dry needling to their potential treatments and grow as a clinician overall. Thank you to Kinetacore and all the outstanding instructors we had this weekend. -Chris
As many of you may have heard, Optim Manual Therapy Fellowship became accredited through both AAOMPT and ABPTRFE. Optim originated in Houston, TX with the 3 cohorts thus far and expanded this past year to Scottsdale, AZ with its first cohort. Optim Manual Therapy currently offers a 1-year COMT program in both Scottsdale and Houston. The program includes 6 on-site weekend long courses covering repeated motions, standardized mobility assessments, Sahrmann's Movement Impairment Syndromes (MIS), and many manual therapy assessment/treatment techniques for each region. Additionally, between classes there are different Medbridge courses assigned in addition to several online case discussion mentoring sessions regularly throughout the year. The COMT program is an excellent way to advance your clinical skills and knowledge and to prepare for the OCS. Should you complete the COMT program, you can then enroll in the Fellowship part of Optim Manual Therapy. If you have interest in joining Optim, don't hesitate to contact me or any of the faculty at Optim. Next cohorts in Houston and Scottsdale are beginning in September! Below you will find a lecture given for the Optim COMT program on Sahrmann's Movement Impairment Syndromes (Foundation and Lumbar Spine). This is just one of many theories we teach our program participants. For more information, check out Optim Manual Therapy's youtube page, Like us on Facebook at Optim Manual Therapy, or check out www.optimfellowship.com -Chris As you may have heard, recently physical therapists in Wisconsin have been allowed to order x-rays. One of the rights that separates chiros and MD's from physical therapists is the ability to order imaging. A significant component of our doctoral education is built upon understanding imaging, so the APTA and subsidies in each state have been working on getting physical therapists the right to order x-rays. While this is a significant step forward in public perception and autonomy as a profession, I have some very strong concerns. If you pay attention to much of the pain science research, you likely are aware of the large number of studies that reveal the lack of correlation between imaging findings and pain. If you take 1000 health people (without pain) off the street and take an x-ray of their lumbar spines, anywhere between 30-70% of them would have spinal stenosis, osteophytes, herniated discs, etc. Simply put we cannot link pathoanatomical findings with pain. So what does this have to do with our ability to order x-rays? Well, one of the things that sets us as physical therapists apart from other health care practitioners is the fact that we base our diagnoses off impairments, not tissue health (or at least that's how it should be). We find weak glutes, we try and strengthen them. We find a stiff lumbar spine, we try and mobilize/manipulate it. The point is the impairments guide our treatment, not the x-ray findings. What I am concerned about, is that with the ability to order x-rays, PT's will suddenly start ordering x-rays on every other patient. Low back pain? X-rays. Knee pain? X-rays. It is inevitable that degenerative conditions will be found on the imaging and likely will be blamed for the patient's pain. In my opinion, this is next to medical malpractice. Some of the most difficult patients to treat are the ones that have their imaging findings memorized and are afraid of "crunching down on a nerve." We must be careful so as not to create these thought viruses in our patients. Now, I absolutely still support physical therapists gaining the right to order x-rays. With our training in being able to screen patients for fractures, infection, cancer, and more, I think it can help to streamline the health care process and save money for our patients. But we must avoid ordering x-rays for every musculoskeletal injury that walks in the door. Remember, the imaging should not guide our treatment, unless managing the condition is outside our scope of practice i.e. a fracture, infection, etc. Congratulations Wisconsin PT's! Show the rest of the country that we won't abuse the power of ordering x-rays and potentially harming our patients! -Chris
 In Physical Therapy school, the highest evidence is literally printed out or emailed to the students so that we leave school practicing the highest level of evidence. Unfortunately, as we begin treating, this information is slowly taken away from us. The astute clinician subscribes to JOSPT, PT journal, social media, and their colleagues to stay on top of the research. Unfortunately, I often feel this information is still not enough. For those of you who have been following our website for a while, you may remember a guest post from Physical Therapist Nick Rainey entitled "Test, Treat, Retest." Recently Nick published an ebook "Research Made Simple for Physical Therapists." The ebook is a quick guide to research for practicing physical therapists, students, residents, and fellows in training. It reviews many of the pertinent physical therapy studies that have been published in the last 10 years. I personally enjoyed the book because of the clinical implications Nick highlights at the end of each journal article. Thanks for the resource Nick! -Jim I had a friend recently with complaints of calf pain that has lasted approximately 6 months. I believe the original injury was after a long run and the "strain" had improved, but never disappeared. He currently only had a sensation of "tightness" when running. As many of you know, anytime an injury lasts more than approximately 3 months, we should start to shift our focus towards the nervous system. I did a very limited assessment in the parking lot after playing a round of golf with him. Multisegmental Flexion and Extension both looked Functional and Non-painful. Sideglides in Standing looked slightly limited loading the involved side. I performed a Passive SLR with a bias of the sural nerve and it recreated his pain with hip flexion. As with any neural complaint, I try to focus my treatment on the spine, but thought he would benefit from neural mobilization as well. Below I will list some of the exercises I would prescribe for a case like this.
In order to ensure end-range with lumbar loading, I recently started prescribing the below exercise as a repeated motion as well. This is another sample video from the Insider Access Page and what we like to teach in Optim Manual Therapy. I instructed him to perform approximately 10-15 repetitions of each of these exercises before and after he went running or did any other kind of exercise; however, ideally, a patient would do about 10-15 repetitions every hour awake as it would likely speed the recovery, lessening the need to do the exercise at all. -Chris
|
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|













 RSS Feed
RSS Feed