- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
Regardless of what setting you work in, you are likely to have to address impairments unrelated to your specialty. If you're in a neuro setting, you'll likely see patients with Parkinson's that have back pain. If you are treating a patient for foot pain with multiple sclerosis, you may have to adjust your exercise prescription. As with any patients, you will have to do a systems review, especially the cardiopulmonary system, for potential contributing factors. Because of this, it is essential that we maintain (and improve upon) our knowledge in different areas. I was recently made aware of a course that John Zapanta, PT, DPT, OCS is teaching, known as Manual Therapy Interventions for the Neurological Patient. If you are looking to increase your competency in treating patients with co-morbidities, this course may be the one for you. -Chris
1 Comment
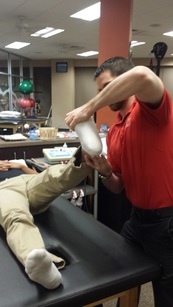
 As many of you may have heard, Optim Manual Therapy Fellowship became accredited through both AAOMPT and ABPTRFE. Optim originated in Houston, TX with the 3 cohorts thus far and expanded this past year to Scottsdale, AZ with its first cohort. Optim Manual Therapy currently offers a 1-year COMT program in both Scottsdale and Houston. The program includes 6 on-site weekend long courses covering repeated motions, standardized mobility assessments, Sahrmann's Movement Impairment Syndromes (MIS), and many manual therapy assessment/treatment techniques for each region. Additionally, between classes there are different Medbridge courses assigned in addition to several online case discussion mentoring sessions regularly throughout the year. The COMT program is an excellent way to advance your clinical skills and knowledge and to prepare for the OCS. Should you complete the COMT program, you can then enroll in the Fellowship part of Optim Manual Therapy. Below you will find a video of Chris using a MWM to address meniscal tears that will improve pain, mobility and function. This is just one of many techniques we teach our program participants. For more information, check out Optim Manual Therapy's youtube page, Like us on Facebook at Optim Manual Therapy, or check out www.optimfellowship.com -Chris In physical therapy school, ACL injuries receive a great amount of attention. I remember learning extensively about the mechanism of injury, ACL anatomy and physiology, biomechanics, and reconstruction protocols. Following an ACL reconstruction (ACLr), the graft undergoes a series of changes to eventually mimic the anatomical ACL. A good protocol stresses the importance of avoiding open kinetic chain activities during the 'middle weeks' of post-surgical rehab because the ACL graft is weakest at this point. In school, I had a difficult time conceptualizing why the ACL is weakest during this phase. Check out the youtube video below which does an excellent job demonstrating how the ACL remodels following ACLr. -Jim
A regular part of your lower quarter exam (and some upper quarter) includes the Slump Test. The purpose of the test is to determine if the nervous system is involved at all in your patient's case and symptom presentation. When performing the Slump Test, we are looking for 3 potential findings: 1. Reproduction of the patient's symptoms 2. Asymmetrical quantity or quality of motion 3. Ability to change the symptoms with proximal/distal motions While I have discussed the potential importance of asymptomatic limitations in nervous system mobility before, I instead want to focus on a different response during the slump test. When I was in school, I was taught that when performing the test, the patient slouches then performs knee extension. The symptoms are increased with ankle DF and decreased with cervical extension in a positive test. While this can be true, I have found some patients have an increase in symptoms with cervicothoracic extension instead. Even though this doesn't fit the normal findings for a "positive test," the fact that a proximal motion changes the symptoms does qualify as being positive for neural tension. The point is we must make sure we follow the 3 rules for determining if a Slump Test is positive, even when it's not our typical positive test. -Chris
 Recently, Dennis Treubig posted an article "ranting" about why he hates the straight leg raise as an exercise on The Manual Therapist (his use of rant). He makes some excellent points about about how it is a significantly inadequate intensity for quad strengthening and the fact that it is more of a hip exercise anyway. He also states that it is useful for special testing and assessing neuromuscular control in patients with LBP. While I may agree with those points, I do not think the exercise should be disregarded altogether. For one, the exercise is functional. If you think about segmental rolling leading with the lower extremity, this is an activity many people do in order to get out of bed each morning. Secondly, I think the exercise is essential for motor control training, not just assessment. When you monitor a patient's pelvic and lumbar position during any open-kinetic chain hip flexion, you may notice anterior pelvic tilt and/or lumbar extension, especially if the patient has back pain. Being able to progressively load hip with open-kinetic chain flexion can be useful for improving lumbopelvic motor control and stabilization. We should be able to flex the hip without excessive mobility occurring in the lumbar spine. I don't want to brush Dennis' rant off as inaccurate, because he definitely makes some excellent points. In no way should we be using the SLR as a strengthening exercise for quadriceps. Additionally, as PT's we need to do a better job prescribing the appropriate dosage for strengthening exercises in general. However, I do think the SLR has some usage as an exercise still for motor control and functional training. -Chris
Hello TSPT Community! We know the words National Physical Therapy Examination cause fear and anxiety in many people. Recently Chris and I were speaking with OPTIM owner Dana Tew regarding how to make the NPTE exam less stressful. Our solution: more resources! Starting this week, OPTIM Manual Therapy Fellowship will make NPTE quizzes for our audience. As a neuromuscular based manual therapy fellowship, many of our questions will be Orthopedic and Neuromuscular focused. We are happy to answer questions and write on specific topics if anyone has questions. The April exam is only a few weeks away & the July exam will be here before we know it! Start studying today and get off on the right foot with our first NPTE Quiz!  OPTIM COMT and Fellowship is now enrolling classes for our 2016/2017 cohorts in Arizona and Houston. Please contact Dana or Jim with questions or comments: E: [email protected] E: [email protected] |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|













 RSS Feed
RSS Feed