- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
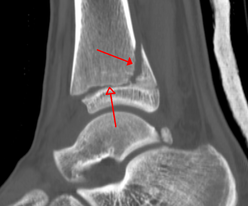
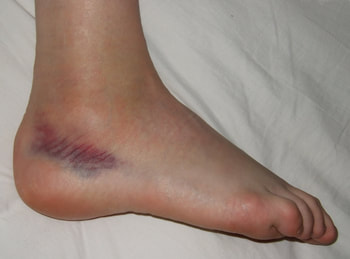
RehabilitationAfter the diagnosis of an ankle fracture has been made, the region is typically immobilized with limited weight-bearing. The severity and location of the fracture contributes to the decision on what level of immobilization is required: open reduction internal fixation, CAM boot, aircast, etc... This timeframe for immobilization typically occurs for 4-8 weeks (factors like osteoporosis and peripheral vascular disease may impact the timeframe). Once radiographic evidence of sufficient healing occurs, the patient often begins skilled physical therapy. Initially, the primary focus will be on reducing swelling and improving joint mobility. This is often done with ROM and stretching exercises, joint mobilization, soft tissue treatment, and modalities. Open-kinetic chain strengthening exercises are typically started once the patient's fear of movement and activity tolerance improved. During this initial acute phase, gait training may be necessary to train the client on how to use crutches, how to maintain appropriate weight-bearing status, etc. As the patient gains mobility and weight-bearing is progressed (based on bone healing), weight-bearing exercises will be progressed. The patient may initially need to perform AAROM exercises in closed-kinetic chain in order to address any apprehension and improve load tolerance, while restoring mobility. Full ankle motion is not required nor expected before weight-bearing is initiated. Once the patient presents with sufficient tolerance, closed-kinetic chain load is progressed further with shuttle squats and calf raises, to full body versions as well. Exercise progression becomes more typical at this point as various methods of loading (lunges, squats, step-ups/downs, etc.). What likely needs to be addressed is stability training in some form to improve reaction and balance when stability is challenged. This can include standing on unstable surfaces, incorporating mental and upper extremity tasks, agility/plyometric training, etc. This progression has no set time table. We have to respect the severity of the fracture, co-morbidities, prior level of function, planned activities to return to and more. Always consider the physician and/or surgeon's prescribed progression, but move your patient through the various phases based on how that specific individual is doing. A patient with a fibular fracture that also suffered a common peroneal nerve injury will likely not progress as quickly as the same fracture without neurovascular insult. There is no set timeframe for recovery from injury, so prepare to be flexible. You may need to incorporate other treatment methods to help move your patient through each step (spinal manipulation, nerve mobilization, therapeutic neuroscience education, among others). Regardless of the contributing factors, the therapists' objective is to guide the patient back to their prior level of function safely. -Dr. Chris Fox, PT, DPT, OCS Want to learn more advanced information to develop your clinical skills and knowledge? Check out the Insider Access Page!
1 Comment
12/8/2021 05:16:14 pm
I like what you said about preparing for neurovascular pain. I need to get a vascular examination of my dad's heart. I'll have to consider seeing the doctor this week.
Reply
Leave a Reply. |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|







 RSS Feed
RSS Feed