- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
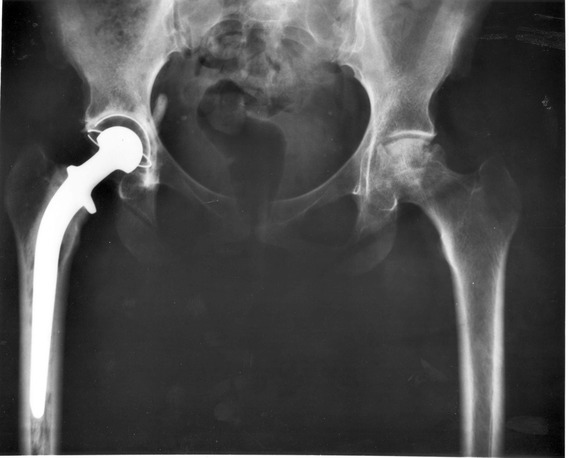
I recently read an article discussing the need for regular follow-ups for patients following THA to determine the potential need for revisions. As many of you are well aware, with the shift in physical therapy practice shifting towards pain science - based, the question of the necessity comes up regarding joint replacements in the first place. The need for joint replacement is supposed to be based on pain, disability, and loss of joint space. The issue with this is there are plenty of people with loss of joint space that have no pain or disability. It is just a sign of aging on an x-ray. Unfortunately, some in our medical community recommend getting joint replacements if pain ever occurs (even if short-lived) if there is loss of sufficient joint space. I've had patients who have come in for hip or knee pain, for prehab to arthroplasty, that I have eliminated their pain and disability, but they think they still need the surgery! Both practitioners and the patient are at fault. Many clinicians are still stuck in the biomedical model, thinking imaging dictates treatment. Many patients think it is best for them to order medical procedures as if they were on a menu at a restaurant. We must do our best to educate our patients on the potential success for conservative management. Given many patients end up having joint replacements anyway, we must address the question of potential revisions. Revisions typically occur due to infection or pain associated with failure of the prostheses. The article I read mentioned the potential need for long-term follow-up with patients who have had joint replacements and performing imaging to assess the integrity of the prostheses and tissues around them. Currently, patients would only follow-up with an orthopaedic doctor if pain returned to the joint. It is suggested regular follow-up should be performed to assess for potential periprosthetic osteolysis and aseptic loosening. The concern is that these findings contribute to osteolysis and potentially mechanical failure. It is a difficulty decision to make as we often forget the risks associated with any surgical procedure at all (infection, complications from anesthesia, etc.). Even if the patient has pain, with the advancements in pain science, should we let imaging findings dictate our treatment. Honestly, I'm uncertain the best method for managing the potential need for revisions. With normal aging, all developmental processes are associated with biological components. After an arthroplasty, a foreign object is introduced to the body and its malfunction may affect normal processes. Typically the way I manage patients with joint pain with a history of replacement is the same way I treat all my patients: treat the impairments. If I find some muscles are weak, I'm going to try and strengthen them. If I find the lumbar spine is not moving sufficiently, I'm going to try and find a way to improve it. I'll try and reinforce my treatment with education of pain science, as well. However, if a patient fails to respond, I will refer them back to the physician. In summary, I'm not sure it's worth the risk of a revision in asymptomatic patients, due to the potential for infection and the role of the CNS in pain perception. But there likely is still a role for revisions in those with pain, if they fail conservative management. -Chris
0 Comments
Leave a Reply. |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|







 RSS Feed
RSS Feed