- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
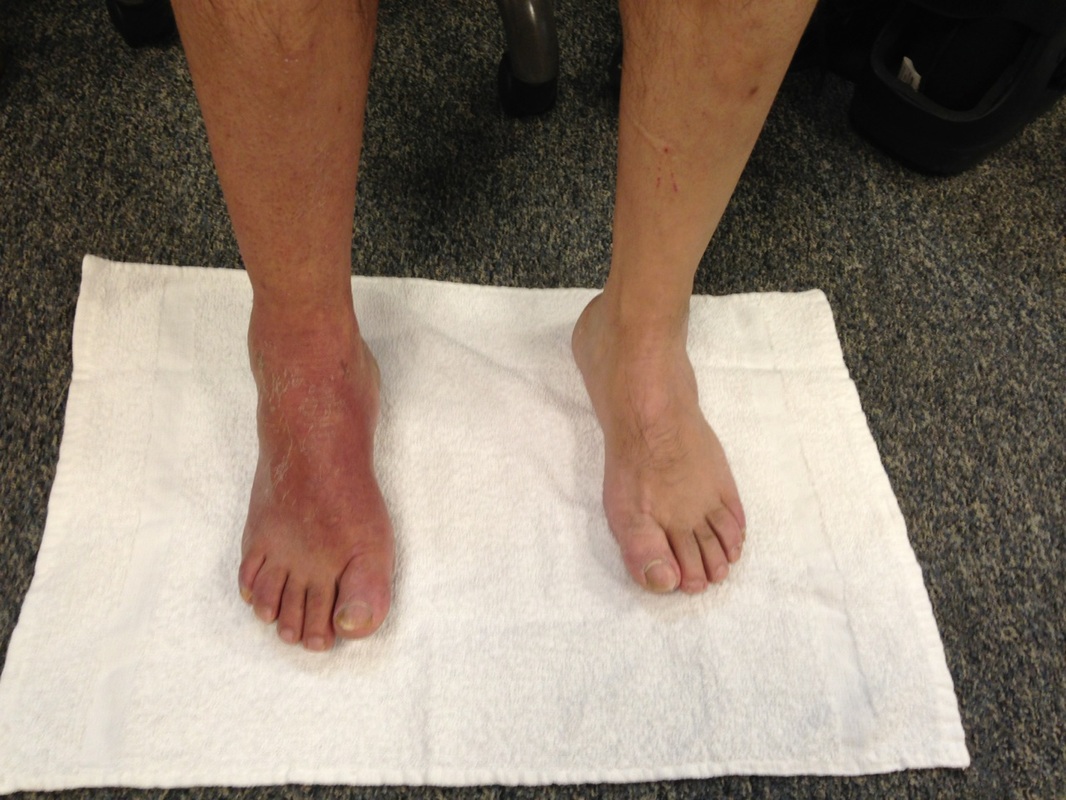
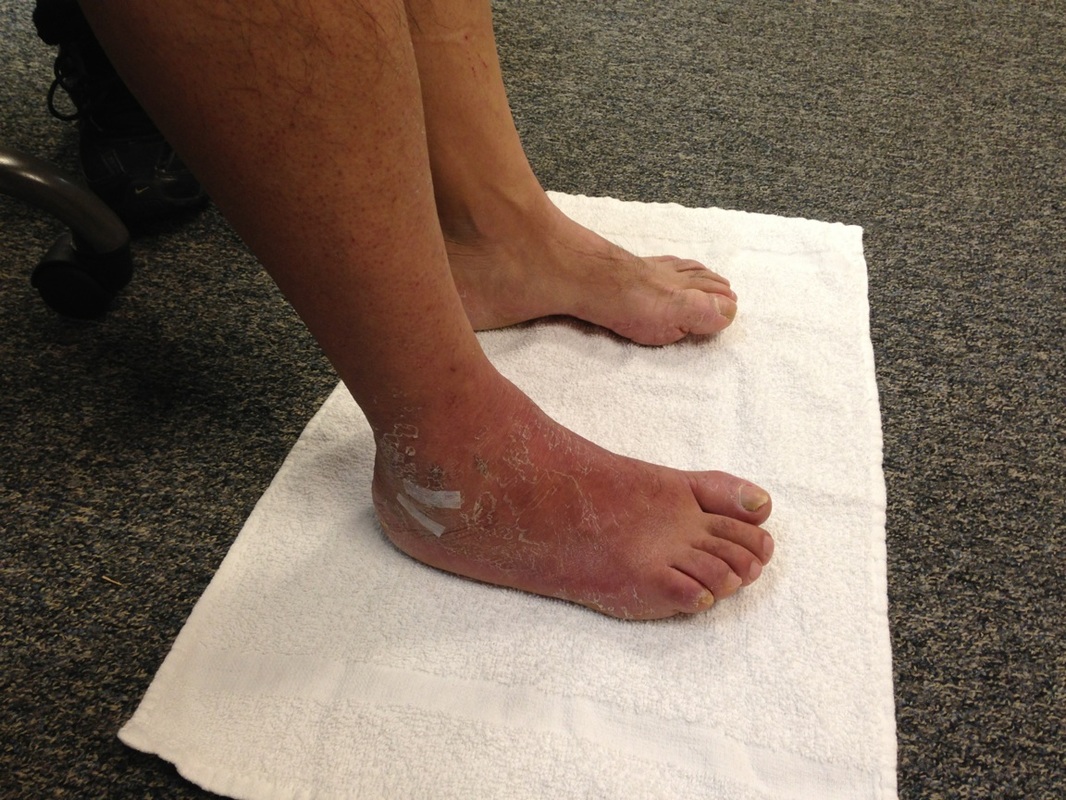
Last week I was evaluating a 50 year old male status post peroneal tendon debridement and repair. The patient had spent 6 weeks in a cast and was seeing me 1-week after cast removal. The two pictures below show how the foot and ankle presented upon initial evaluation. My initial differential diagnosis included: 1. normal foot, 2. infection, 3. CRPS. Further inspection revealed signs of skin trophic changes, swelling, pain, hypersensitivity to light touch, nail bed changes, coolness of the lower limb and difficulty initiating movement. The patient denied constitutional signs and symptoms- fever, chills, headaches, night sweats. The incision appeared to be healing normally. He had limitations in ankle ROM and strength. Interestingly, the patient had a positive SLUMP test with intermediate dorsal cutaneous nerve bias (branch of the superficial peroneal). The patient's symptoms had centrally sensitized! After being in a cast for 6 weeks with high levels of pain, the CNS forgot how to interpret normal sensation and movement of the foot. On the initial evaluation, I performed a thoracic manipulation to stimulate the autonomic nervous system as well as performed common peroneal nerve glides. Additionally I prescribed the ankle alphabet and towel scrunches bilaterally to facilitate bloodflow and movement as well as promoting small amounts of weight bearing. I chose to perform each exercise bilaterally so that the patient would receive neural overflow from the intact side. Additionally, I gave ample education to the patient regarding the nervous system and pain science. Even in surgical cases, remember that the cause of dysfunction may be distant from the site of injury! More pictures and progress updates to come. -Jim Check out our Insider Access page to see specific testing for lower extremity nerves! Like this post? Check out other posts by TSPT.
2 Comments
tommie
4/16/2015 02:31:07 am
Good one Jim! Just got a fresh one of these myself Tuesday. She had a brunstrom procedure done w/ peroneal groove deepening. If they were in a boot don't forget to check for an iliac upslip on that side. My pt had a massive one. Also manip (or mob) L4/5 L5/S1 for the next I physiological response.
Reply
Jim
4/17/2015 02:24:15 am
Tommie,
Reply
Leave a Reply. |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|






 RSS Feed
RSS Feed