- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
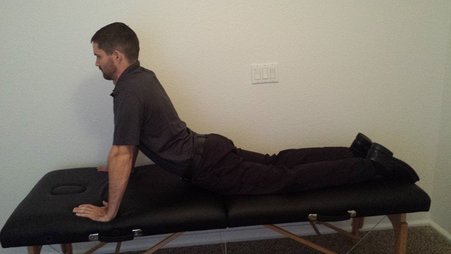
Recently, I have been reading the McKenzie texts in order to gain a better understanding of the foundation material. I had previously gotten my education on utilizing repeated motions from The Manual Therapist and then developed my practice through clinical implementation since then. Typically, when people think of McKenzie, they simply think of everybody doing lumbar extensions. After going through the lumbar spine text books, it is refreshing to see the standardized approach in the McKenzie system. However, I would argue the school of thought doesn't address the lumbar spine enough. The McKenzie system is very anatomy driven. The theory is built off of addressing disc herniations, radiculopathy, and more. While each patient is expected to be taken through a standardized assessment of repeated motions in various directions, should no significant signs of lumbar involvement be present, the lumbar spine may not be addressed. For example, one of my former students and I had a patient with all signs of an acute meniscus tear, confirmed with imaging and testing. He did not respond to any local repeated motions but had complete elimination of pain with spinal repeated motions. With a personal example, I had signs of either a neuroma or metatarsalgia that responded perfectly to repeated motions in the lumbar spine. An experienced McKenzie therapist may have addressed the lumbar spine in examples like these, but it doesn't fit the typical diagnostic criteria. With what we know about "double crush syndrome" and pain science, we must address any potential perceived threat in the body. Typically, one of the biggest drivers of neural sensitivity comes from restricted spinal mobility. In pretty much every injury, the spine should be assessed for mobility deficits and addressed. Otherwise, long-standing "calf strains," meniscus tears, trochanteric bursitis and more may go without improvement. -Dr. Chris Fox, PT, DPT, OCS
4 Comments
chad
9/21/2016 01:28:44 pm
I like the article and I can see where your opinion comes from but in my opinion, McKenzie does not focus so much on anatomy in regards to treatment but it does focus on anatomy in regards to patient education and finding that "patient buy in". The anatomy may be the trick to dec. their threat of pain with motion. I use it as my primary method of treatment and move to something else if I do not have any luck.
Reply
Hi Chad,
Reply
9/28/2016 05:55:13 am
Your thought about the topic is correct. I think that people need to think about it, in the same way you do or what you have expressed in the blog. I really like your idea and your presentation skill. Nice work.
Reply
Chad Shafer
9/28/2016 11:45:14 am
I totally agree with you Chris and I enjoyed the article. I think with the MDT approach, if you are looking for a DP and explaining why it works can go either way. I definitely agree that the pure MDT approach may instill fear about flexion, but I always find myself saying "flexion is not bad for you, but lets try a direction that you never move in to make your pain better."
Reply
Leave a Reply. |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|







 RSS Feed
RSS Feed