- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
During one of my recent mentoring sessions for my fellowship, we saw a patient that had plateaued in progress. The patient was being seen for right upper extremity pain. The patient initially presented with pain that was associated primarily with cervical radiculopathy signs, such as bakody's sign, (+) cervical distraction test, (+) ULNT, etc. The patient initially responded great to PT as the radicular signs completely normalized. However, some right anterior shoulder pain remained that presented with signs of symptoms of shoulder dysfunction (anterior glide medial rotation syndrome, weak shoulder ER, restricted IR mobility, etc.). We gave him a few exercises to address these deficits. After a couple weeks, the pain in his shoulder had not changed and we had to decide the next course of action. The patient's initial reaction was to "give up and live with the pain." We initially talked about the possible benefit of an injection to address the pain, however, that was when our discussion switched to plan of care directly regarding PT. Upon examination, the patient still had restricted inferior GH capsular mobility, shoulder ER strength and scapular strength deficits. While the pain had not improved, the impairments had, but still had dysfunction remaining. When I first came out of school, I may have referred this patient back due to lack of progress, but with the deficits remaining, I would recommend continuing PT. His pain at this point still has impairments associated with it that can be addressed by PT, so we modified his HEP to focus on these strength and mobility deficits. Don't be so quick to give up on a patient's rehab. It is easy to become concerned when the patient isn't responding as we had hoped, but that is why it is essential to regularly evaluate the patient's progress in strength, mobility, flexibility, etc, instead of simply referring the patient back. It helps us track progress and helps the patient understand how they are responding as well. A change in the treatment plan or perspective may be necessary, or continue along the path the patient is currently on if progress is being shown. -Dr. Chris Fox, PT, DPT, OCS
1 Comment
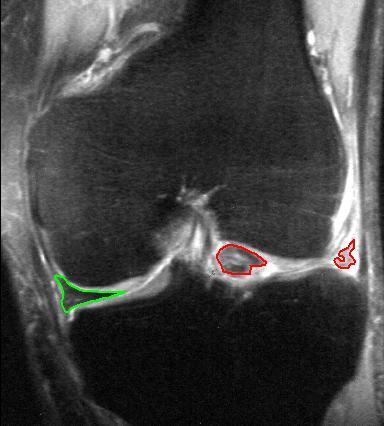
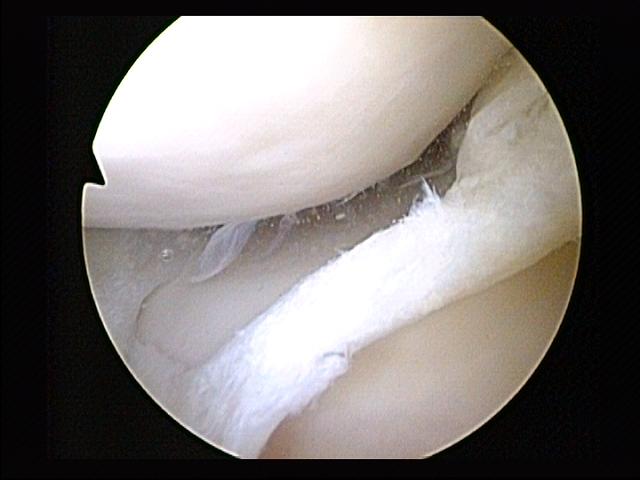
 How many of you offer annual wellness screenings? How many of you would like too? As physical therapists, many times we get so stuck on offering reactive services (after injury) that we forget how valuable we really are! Think about it, we study the human body and how to move properly. Yet, as PT's we do a poor job of describing what we do and how much value we bring. This brings up the idea of offering annual wellness screens. After all, people visit the dentist, their doctor, and their accountant every year but don't get a check up on their bodies and they have to live in them everyday. We must get out of the thinking of PT only as reactive and start thinking about how much more we can help people. How many people say to you they start a fitness program only to get injured and have to stop? Or the desk jockey that says they used to be an athlete but now always feels stiff? These are perfect times to bring up how easy it would be to do an annual screen to prescribe suggested mobility or strengthening exercises to improve their condition and prevent future injuries. So what do you include in an annual wellness screen? Well, there are many things you could include but remember we are movement specialists so I would make sure you include major movements such as the overhead squat, shoulder functional ER/IR , lumbar ROM, and various breakouts based on the dysfunctions. You also want to tailor the screen to the person's individual activity. If they are a runner include some single leg squatting and hip extension screens. If they are a tennis player look closely at their overhead stability and mobility. This will ensure that the person you are screening feels the value in what you are doing for them. Remember that as PT's we offer a service and we bring value to people. Start to educate yourself on an elevator pitch and really think about some of the other services you can offer your current patients or future patients. We can do a lot more for people to help them. Dr. Brian Schwabe, PT, DPT, SCS, COMT, CSCS With this past month's JOSPT, an updated Clinical Practice Guideline (CPG) for Knee Meniscus and Articular Cartilage Lesions was released. Meniscus tears and cartilage lesions are commonly seen in the physical therapy setting. Once thought to require surgery, significant research has since revealed that outcomes are similar whether you have had surgery or physical therapy about a year later. While being able to identify the potentially injured tissue can be beneficial, treating the impairments remains the basis for intervention. However, because of the research that has been accumulated in managing meniscus and articular cartilage injuries, it is still recommended that we identify when these structures may be involved.
Now, some of the research for treating these injuries conservatively is based off of post-surgical management. A lot of the rehab is what you would expect: start with progressive active and passive ROM training and weight-bearing, followed by strength training in open- and closed-kinetic chain and neuromuscular training of lower quarter. Those are generally vague component to rehab but can be highly effective. Of course, not all cases are "text book." Sometimes (or often), the patient's perspective of what the injury is, or what they think it is, is more important than anything. It is extremely beneficial to educate the patient on the current pain science research, the lack of correlation between pathoanatomical injuries, and the success of conservative rehab for meniscus/cartilage injuries. The importance of progressive loading cannot be overstated. While part of the CPG, using regular and progressive loading can have both mechanical and psychological benefits. There is some research out there that high repetition, low load exercise can be beneficial for cartilage repair. On the biopsychosocial side, progressive loading of the injured area can address some of the fear and apprehension associated with injury. Either way, the main message to take away is that physical therapy can be a possible treatment for meniscus or articular cartilage lesions, based on the recent CPG's, mechanotransduction, and/or psychological benefit. -Dr. Chris Fox, PT, DPT, OCS Today's post is from Meredith Castin of The Non-Clinical PT. Thanks Meredith!
You’ve probably heard plenty of grumbling about how the times are a-changin’ in the PT world. Reimbursements are falling and salaries are stagnant at best. Perhaps your loans are looming at epic proportions and you wonder how you’ll ever land a job where you’ll pay them off, much less make a solid living in the process. Here’s the thing. Lots of PTs are extremely successful in today’s healthcare climate--they’re just changing their approach by seeing themselves as a hot commodity and putting themselves out there as soon as possible. If you spend any time online (which you must, if you’re following this awesome website and reading this article), you’ll notice that some PTs are just savvy with technology. They’re putting themselves out there and they’re getting noticed. They’re interacting with influencers online and they’re making names for themselves before they’ve even finished PT school. They’re creating their own online brands for themselves, and you bet your bottom they’ll be the ones getting snatched up for the best jobs when they graduate! Frankly, I was not that person during school, and I regret it. I waited until I’d been out of school for four years before I even started to make a name for myself online, and I’m writing this article so that you don’t make the same mistake. Start That Website: If you’re a PT student or a new grad, you need to start a blog or a website--whatever you want to call it. It’s easy. Just hit up Wix or Squarespace, or Wordpress (that’s my fave and what I use for TheNonClinicalPT.com), and it’s blindingly simple to get things started. But here’s an inexpensive class to de-mystify Wordpress, just in case you like to understand all the bells and whistles, and get an idea of how to maximize your efforts. I do recommend taking a basic course. In any case, writing about a topic for long enough eventually makes you the expert on that topic. Whether you opt to stay in patient care or leave patient care to leverage your physical degree in a non-clinical career, you need to write about something at least loosely related to physical therapy. Write about what interests you, and what comes naturally. You’ll never find me writing about tibiofibular mobilizations because I don’t find that topic inspiring. I write about non-clinical careers about PTs because that’s what I know. As for you, you can talk about studying success, the trials and tribulations of being a student, careers, finding good clinicals, technology, networking, ballet, badminton, or whatever else you feel compelled to cover. Notice how I included ballet and badminton? When I first started writing, it was at the behest of my co-worker (at the time), Brett Kestenbaum, DPT. He wanted to start a website for new physical therapists and I was like, “I don’t really like being a PT. I don’t even know if I want to keep treating patients much longer. Why would I create a website to help new grads? What if I have nothing to offer? WHAT WILL I WRITE ABOUT?” Well, I figured, at least I knew I liked writing, so I went for it, and I wound up writing about the one thing I did know--how to get the most out of my degree without burning out. I didn’t enjoy treating full-time, so I covered topics about working per diem, preventing burnout, and alternate paths for physical therapists. Lo and behold, after I started writing about my favorite topics--leaving patient care and leveraging my degree to become a writer, I found that people started seeking me out to do exactly that: write. It was a wonderful feeling to finally build a career around something I love. And it wound up being my “golden parachute” for when I really did decide I needed to leave patient care behind. That’s why you need to write. You can’t predict what will happen to you. You might want to leave patient care, or you might want to land a dream job working with professional badminton players. Or dancers. If you write about dancing, even while you’re still in school, you know a hell of a lot more about dancing and PT than 95% of the public. And as you gain experience, that number will climb to 99%. And with your name out there as being the expert about dancing and PT, you’ll land those dream jobs working with ballet companies much more easily than if you were too lazy to start a blog. What If I Really Suck at Writing? It’s OK...if you really hate writing, or really suck at it, you have a few options:
The main point is that you’re putting yourself out there. When you’re a student PT or a Fresh PT and you’re competing with all the others to make a name for yourself, you simply have to do something special to stand out. Otherwise, you might find yourself ten years into your profession, wanting something new, and having to start from scratch when you’re already feeling burned out. I guess I probably should really have called this article “Why Every PT Student Needs to Put Himself or Herself Out There.” But that doesn’t really have the same ring now, does it? Author: Meredith Castin, PT, DPT (The Non-Clinical PT) Follow her on: Facebook | LinkedIn | Twitter | Instagram TheNonClinicalPT.com  If you work in a sports medicine environment like I do, then chances are you are getting quite a bit of ACL reconstructions this time of year. With ski season in full swing, unfortunately, many end up with ACL tears. However, a good majority of these patients are recreational skiers that like to dabble in many other sports. I recently had a few patients who asked about return to running following this surgery. This is always a time when I like to educate the patients on what I want to see from them to get them back to running. By establishing some criteria early on, it allows the patient to get in the mind-frame of what they need to accomplish as well as setting some goals. However, there are many different opinions to what should be established for return to running post ACL. From my perspective, besides time frame and MD clearance, I like to see a few biomechanical considerations. For example, I like to have a patient single leg squat a minimum of 10-15x under control with good form. What do I consider good form? Well, I often use the single leg stepdown criteria that has been established in some of the literature. Another thing I will look at is core stability. Specifically, I typically like to use a front plank with reciprocal arm drivers. The idea being that this test will look at rotational control when a patient is mimicking the arm swing during running. Again, a general time frame I use is at least one minute. Lastly, I like the reverse lunge for looking at great toe extension and hip extension. Remember that running is a full body exercise and it requires lots of moving parts. While the above is not completely comprehensive, it gives a good starting point to look at with running. Lastly, if you like this article, check out the post I made for New Grad Physical Therapy on some of the above criteria and more with pictures. Or check out our Insider Access page where I go into very detailed return to sport criteria and exercises for multiple different sports and movements, such as return to lateral agility. - Dr. Brian Schwabe, PT, DPT, SCS, COMT, CSCS Join Insider Access Today!Thoracic Outlet Syndrome: How is it Defined?Thoracic outlet syndrome (TOS) can be defined as a compression of the neurovascular bundle as it passes between the neck and axilla. Common compression points are between the anterior and middle scalene, between the first rib and clavicle, underneath the pectoralis minor, or potentially the presence of an extra cervical rib. Patients with thoracic outlet syndrome typically present with forward, rounded shoulders and a history of repetitive overhead motion. Both the neural and vascular structures can become compromised, but >95% of all cases are neurogenic. If you are suspecting a patient with neurogenic TOS cluster your TOS tests results with other neuro-dynamic tests. TOS Explained by Dr. Robert Thompson at Washington University in St. Louis How I Treat Neurogenic TOS: A Case Study ExampleEach individual case will have slight variations, but the examination section will be similar for each person My Personal Experience with Venous TOSIn 2010, my entire right arm started to swell. I went to the doctor and initially was prescribed antibiotics for MRSA. I had been paint-balling 2 days prior to the incident and had a few open wounds that were potentially infected. The doctor said to follow up in a few days if I did not improve. My arm continued to swell and became even worse with activity. At the second visit, I was told to go to the hospital to get a venous doppler for a suspect DVT. The doppler revealed a ~4 inch blood clot in my subclavian vein. I was immediately admitted to the ER, placed on blood thinners, and underwent a surgical procedure to remove the clot. CLICK BELOW TO CONTINUE READING -Jim Heafner PT, DPT, OCS Want to learn more from TSPT?
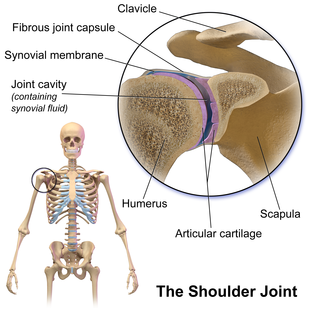
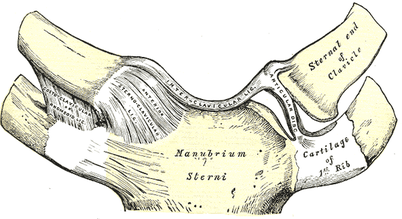
This past week I had a patient that presented with left upper quarter pain following a traction injury to her left arm as her dog yanked her arm forward. The pain was located over her left clavicular region and anterior to left scapula. My examination revealed hypomobility over her left ribs 2-3 and left sternoclavicular (SC) joint as her primary restrictions (both of which reproduced her pain when assessed). She has made excellent progress just in the treatment from the first day with joint mobilizations of the SC joint and and ribs. With reflecting upon this patient, I thought it would be great to review some of the anatomy and arthrokinematics for the SC joint. Anatomy of Sternoclavicular Joint The SC joint is made up of the medial end of the clavicle, the manubrium and an articular disc in-between. It is important to understand that the sternoclavicular joint is a saddle joint. It gets its name from the shape as it has a concave surface in one direction and convex in another, like a saddle. The medial aspect of the clavicle is concave anterior-to-posterior and convex superior-to-inferior. The manubrium has the reciprocal joint surface. The result is that with protraction/retraction, the sternum rolls and glides anteriorly and posteriorly, respectively speaking, and with elevation and depression, the clavicle rolls and slides opposite (roll superiorly and slide inferiorly with elevation; opposite for depression). Additionally, there is some posterior rotation of the clavicle that occurs with elevation and anterior rotation with extension. When it comes to assessing and treating joint restrictions in the SC joint, I try to keep it simple. Assess the mobility in each direction and mobilize into the restriction. It's possible you'll note some hypermobility in a certain direction (you don't want to increase mobility there). Often, you will note that the restricted aspect of the joint may correlate with physiological motion deficits in the shoulder; however, that is not a rule of presentation. To make matters simpler, stick with finding the restricted direction and mobilizing it. For more information on the anatomy and biomechanics of the SC joint, check out the videos below! -Dr. Chris Fox, PT, DPT, OCS
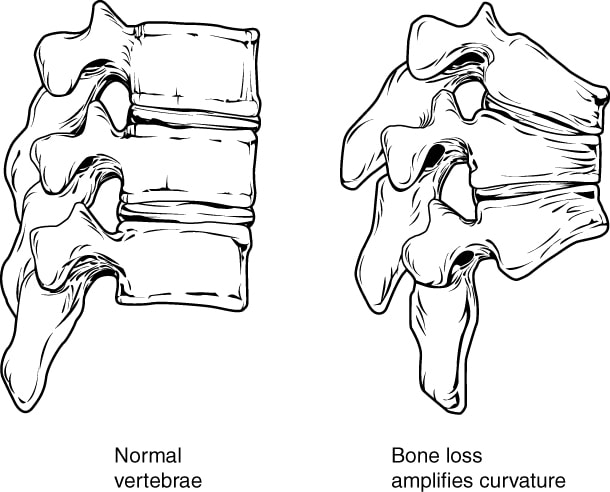
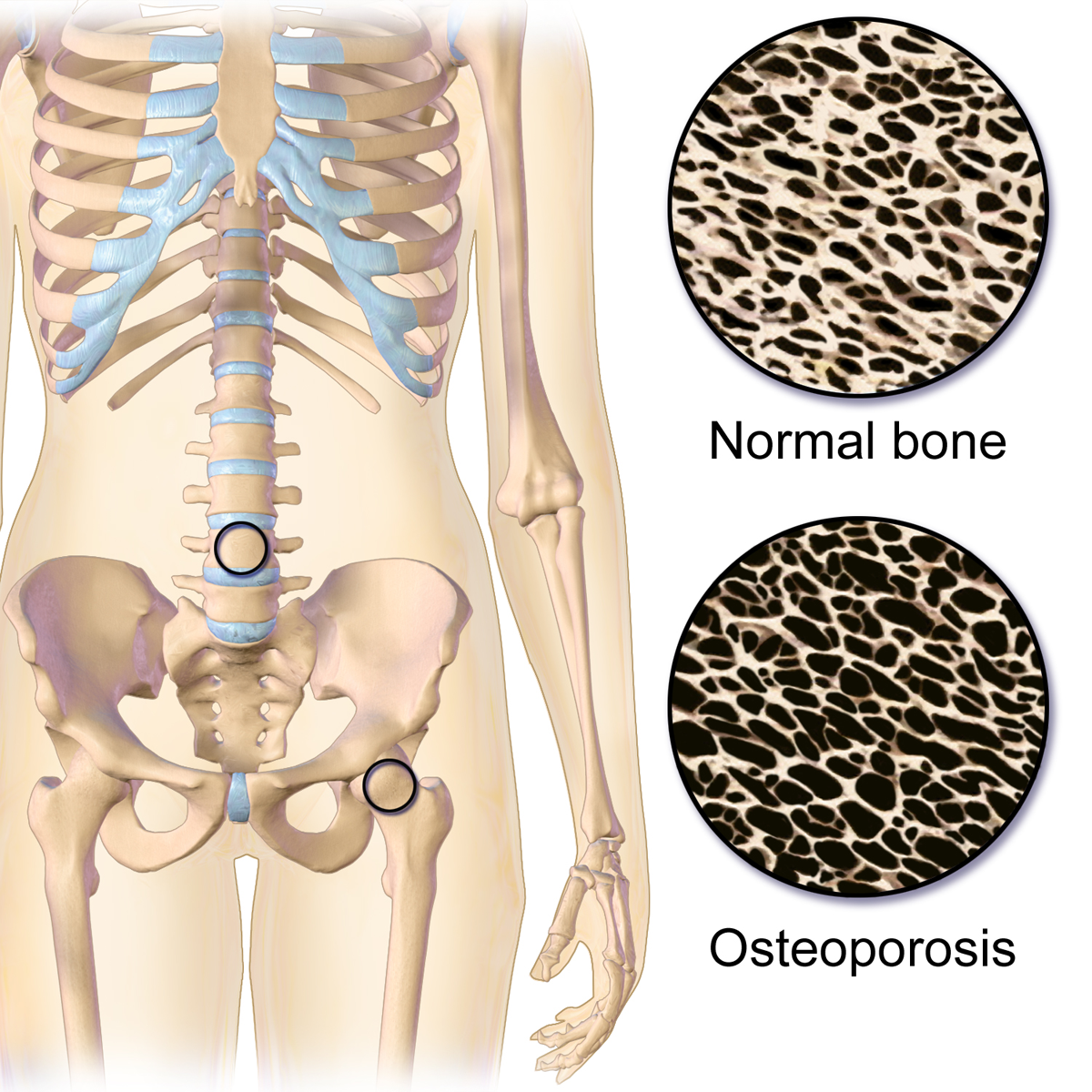
 Aligning with the theme of this month, overhead athletes, today we are going to talk about the biomechanics of the tennis serve. The tennis serve is one of the most complex movements in regards to mechanics. With the amount of force required to generate power from the ground up, it is truly a movement that requires the full kinetic chain. Depending on what research you read, the tennis serve is broken down into approximately 8 stages. Stage 1- Body Positioning: The idea with this phase is to start to properly set up the body for force generation. Stage 2- Ball Release: The idea with this phase is to toss the ball at 100 degrees of abduction and just lateral from overhead. The importance of ball release positioning is that it will effect the GH positioning and how much shoulder abduction is required. While it may seem insignificant, this is one of the most important phases to prep the body for the success of the tennis serve. Stage 3- Loading: This phase is focused on building power through the legs. There are two ways athletes take on this phase.... One way is the "foot up" approach which allows greater vertical forces. For those athletes that prefer the "foot up" approach during the loading phase, they require significantly more eccentric control for the landing. For those athletes that prefer the "foot back" approach, they require increased front knee extension. Therefore, those with quadricep tendon or patellar tendon issue may struggle with this approach at times. The benefit of this approach is a wider base of support which allows for increased squat depth. Stage 4- Cocking: This phase is important for developing max potential energy before impact. Biomechanically, the shoulder and pelvis will tilt laterally, the spine will move into a hyperextension, lateral flexion, and ipsilateral rotation while the shoulder abducts 100 degrees and externally rotated with the elbow flexed and wrist extended. Quite a bit of shoulder stability is required from the supraspinatus, infraspinatus, subscapularis, biceps, serratus anterior, and left internal oblique (right handed hitters). Stage 5- Acceleration: This phase is important for transitioning into forward movement of the serve. Speed is dependent on the previous four stages. The internal rotators of the shoulder (pec major, lats, subscap) and the trunk muscles are the primary movers in this phase. Furthermore, there is peak activity of the gastroc and quadriceps towards the end of this phase. Stage 6- Contact: This phase determines the ball velocity which is dependent upon the amount of shoulder internal rotation and wrist flexion. Additionally, the shoulder abduction angle at contact is typically around 100 degrees, in addition to the significant lateral tilt of the trunk. Stage 7- Deceleration: Similar to the baseball throw, the deceleration phase is the most forceful due to the eccentric contraction of the post cuff, serratus, deltoid, and erector spinae muscles. Stage 8- Finish: Lastly, the finish is the braking forces of the tennis serve which requires complete stop of the movement to get ready for the next shot. This is the phase which requires the most lower extremity eccentric forces. So why is this important? Understanding biomechanics of the positions our athletes get into can help us address their specific complaints. Additionally, it helps us connect to our athletes to be able to speak the same language as them to instill confidence in our ability to understand what they do in their sport. - Brian Schwabe, PT, DPT, SCS, COMT, CSCS See more from TSPT: If you are looking to improve your clinical efficiency, a simple place to start is the intake paperwork. The intake forms often provide the patient's medical background, outcome measures, etc... AND hopefully gives a glimpse into the patient's own description of their symptoms. This is essentially a snapshot of their subjective history, which guides you into specific objective measures. In this post, I outline the power of language from the intake paperwork and my strategies to maximize my efficiency prior to EVER meeting the patient. The Power of LanguageA patient's language provides significant insight into the underlying cause of their problem. For example, if I am reviewing a new evaluation's paperwork for someone who has experienced chronic low back pain for the past 10 years, I am interested in their current thoughts about their systems. If the pain has been present for 10 years, what other interventions have they tried...? do they believe it can get better? If they perseverate on past surgeries, anatomical degeneration, their dog that passed away when they were young, and getting fired from a job 6 years ago, I can draw conclusions regarding biopsychosocial factors are influencing their low back pain. This same patient has likely uses language that reinforces their current symptomology. The language is engrained in the patient's neurology and likely includes thought viruses and f.e.a.r (false evidence appearing real). Thought Virus: “A thought virus is a negative or limiting belief. Often times, a thought virus is generalization or a misrepresentation that was once drawn from experience but is now inaccurate because of its separation from current context as well as evolution of knowledge and understanding. The danger in thought viruses is that, because they often contain some truth or they are partly true in some contexts, people are less likely to question their validity.” Heafner Health Intake QuestionsAs part of my intake paperwork at Heafner Health, I have all patients answer the questions below. With these questions, I want to know why someone is coming to see me, what activities they are unable to do, and approximately when their symptoms began. While I am looking at the objective data with each question, I am also investigating the specific language they use to describe their problem. Their answers provide insight into their perception of injury, fear avoidance to movement, and what they believe causes their issues. When someone answers the intake paperwork, I am merely trying to gather raw data that will then be confirmed or denied during the initial evaluation. Each question is a sliver of the entire pie that creates the framework of their current injury. Reviewing my questions above, here are my thoughts to the answers for a patient I treated a few weeks ago: Questions 9/10: What is the primary issue that brings you in today? This patient identifies his bulging discs as the primary issue that brings him into the clinic. Typically, when someone writes 'bulging discs,' I make a mental note to educate the patient regarding low back pain and disc degeneration as this is a common misconception. Specifically, I provide education in the form on an analogy. A common analogy I use for disc degeneration is the 'wrinkles on the inside' concept, which discusses that we age internally just as we age externally! Despite his anatomical answer to question 9, he acknowledges that his osteoarthritis is 'age appropriate' in question 10. I will still discuss disc degeneration, but hopefully it will be a welcomed conversation. Question 11: As a result, I am having difficulty with? This particular client is not having too much difficulty with specific activities, but rather wondering the difference between 'good' and 'bad' movements. His response is positive because likely he has a low level of overall irritability. Other patient's respond with detailed language that insinuates a fear of movement. Based on his response, I already anticipate a quick return to full activity. For question 11, my focus will be providing education on posture and movement. Newer studies on posture and pain, have demonstrated there are no 'good vs. bad movements.' My education would go as follows: "As humans beings we are designed to move. You have probably heard the quote 'movement is medicine.' It is absolutely true! All movements are great as long as our brain and body are adequately prepared for the movement! To live healthy lives, we must have the capability to explore the bad posture positions equally as well as we can perform the good postures." Question 12: This answer reaffirms his low level of irritability! I am good to proceed to Question 13. Question 13: When did your symptoms begin? This patient provides two answers to his onset of symptoms, either recently or decades ago. From his response, I can gather that he is experiencing a recent onset of a chronic injury. As someone who treats the neuromusculoskeletal system, I am interested in both answers. His older injuries and how he managed them will directly play into the management of this recent onset. Most importantly, I want to know how his January 1969 injury plays into his current symptoms. There must be a strong connection to his original injury if he reports the month the event began roughly 50 years ago! This answer is worth exploring in greater detail during the subjective interview. Closing ThoughtsThe words we use and how we use them have an immeasurable impact on a patient. If ‘thought viruses’ have the potential to worsen a patient’s prognosis, the opposite must also be true. Learning to evaluate a patient's language even before they arrive at your clinic can prepare you for the upcoming evaluation. As health and wellness providers, the ability to understand someone’s needs, and tailor one’s language toward these needs, can significantly influence the outcome of their situation . Author: Jim Heafner PT, DPT, OCS More from The Student Physical TherapistComing out of physical therapy school, one of the many things I was uncertain about was when it was okay to manipulate a joint in the geriatric population. Obviously, some of the usual standard contraindications are included: fracture, instability, etc. However, bone density deficits can be difficult to identify in evaluations as patients don't always have recent (or sometimes any) knowledge of their bone health. To assess bone density, a patient has a DEXA scan performed. The standard deviation then plays a role in assessing how severe any density issues may be. If the score is less than 1 standard deviation from the norm, it is still within the normal range. If the score is within 1-2.5 standard deviations of the norm, the area is identified as osteopenic. If the score is greater than 2.5 standard deviations from the norm, the area is osteoporotic. Should a patient present with either osteopenia or osteoporosis, it is not recommended to manipulate the joint. It would be wonderful if it was as simple as that. However, not every patient knows if they have poor bone density. They may not have gotten a recent DEXA scan. Because of this, we should consider other factors that may contribute to poor bone health and lead to density issues: long-term corticosteroid use, cancer, older age, female, poor nutrition, and more. Should a patient have any or several of these factors, they may very likely have bone density issues as well. This is further evidence that a thorough evaluation (especially subjective history) is essential in patient management. Their history may indicate the safety with joint manipulation. -Dr. Chris Fox, PT, DPT, OCS Looking for advanced sports and orthopedic content? Take a look at our BRAND NEW Insider Access pages! New video and lecture content added monthly.
|
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|



















 RSS Feed
RSS Feed