- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
Patient's often present to the clinic with pathoanatomical diagnosis'. For example, they may have a referring diagnosis of a rotator cuff tear, hip bursitis, or sciatic nerve pain. While this information can often guide us to the region involved, it rarely sheds light on the underlying cause of the problem. As a profession, it should be our goal to be experts in treating the movement dysfunction. Do you find yourself treating local anatomy or searching for underlying movement problem?
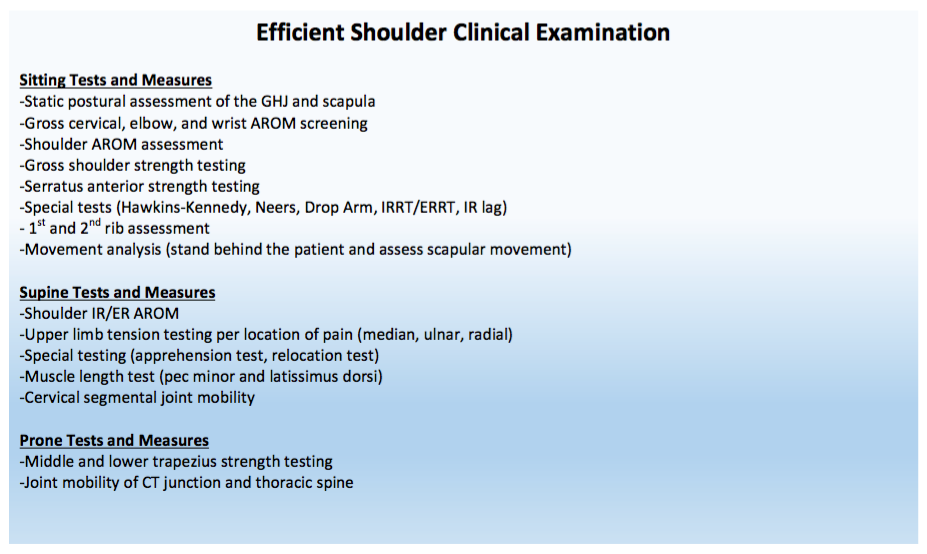
In my recently published clinical booklet, 'The Guide to Efficient Physical Therapy Examination,' I stress the importance of having a movement based examination process. For example, during a shoulder evaluation, the majority of special tests taught in physical therapy school assess specific tissue dysfunction (biceps tendinopathy, labral tear, etc...) Additionally, many of these tests have poor statistics. Remember, we need to assess movement dysfunction - not anatomical tissue dysfunction! Below I have included my step-by-step shoulder examination. In my standard exam, you will not see glenohumeral joint mobility testing or strength testing of the rhomboids. These tests are typically not indicated. The glenohumeral joint is built for mobility, unless the individual has clear mobility deficits (i.e. adhesive capsulitis), joint mobility is usually not an issue. Additionally, many people rest in scapular downward rotation and demonstrate strong and dominant rhomboids muscles. While your personal examination may include or exclude certain steps, always remember that we are movement specialists and your testing should be guided by movement impairments.
-Jim Heafner PT, DPT, OCS
1 Comment
Rofida shokry
9/6/2019 04:07:23 am
First of all,thanks doc for all this amazing information and for sharing it with us .I want to know if you can name a shoulder course like the other courses to learn more from you
Reply
Leave a Reply. |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|







 RSS Feed
RSS Feed