- Home
- About Us
- TSPT Academy
- Online Courses
-
Resources
- Newsletter
- Business Minded Sports Physio Podcast
- Day in the Life of a Sports PT
- Residency Corner
-
Special Tests
>
-
Cervical Spine
>
- Alar Ligament Test
- Bakody's Sign
- Cervical Distraction Test
- Cervical Rotation Lateral Flexion Test
- Craniocervical Flexion Test (CCFT)
- Deep Neck Flexor Endurance Test
- Posterior-Anterior Segmental Mobility
- Segmental Mobility
- Sharp-Purser Test
- Spurling's Maneuver
- Transverse Ligament Test
- ULNT - Median
- ULNT - Radial
- ULNT - Ulnar
- Vertebral Artery Test
- Thoracic Spine >
-
Lumbar Spine/Sacroiliac Joint
>
- Active Sit-Up Test
- Alternate Gillet Test
- Crossed Straight Leg Raise Test
- Extensor Endurance Test
- FABER Test
- Fortin's Sign
- Gaenslen Test
- Gillet Test
- Gower's Sign
- Lumbar Quadrant Test
- POSH Test
- Posteroanterior Mobility
- Prone Knee Bend Test
- Prone Instability Test
- Resisted Abduction Test
- Sacral Clearing Test
- Seated Forward Flexion Test
- SIJ Compression/Distraction Test
- Slump Test
- Sphinx Test
- Spine Rotators & Multifidus Test
- Squish Test
- Standing Forward Flexion Test
- Straight Leg Raise Test
- Supine to Long Sit Test
-
Shoulder
>
- Active Compression Test
- Anterior Apprehension
- Biceps Load Test II
- Drop Arm Sign
- External Rotation Lag Sign
- Hawkins-Kennedy Impingement Sign
- Horizontal Adduction Test
- Internal Rotation Lag Sign
- Jobe Test
- Ludington's Test
- Neer Test
- Painful Arc Sign
- Pronated Load Test
- Resisted Supination External Rotation Test
- Speed's Test
- Posterior Apprehension
- Sulcus Sign
- Thoracic Outlet Tests >
- Yergason's Test
- Elbow >
- Wrist/Hand >
- Hip >
- Knee >
- Foot/Ankle >
-
Cervical Spine
>
- I want Financial Freedom
- I want Professional Growth
- I want Clinical Mastery
|
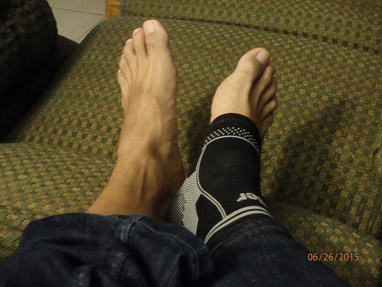
How do we know when to discharge our patients? Is it when their pain goes away? Is it when they reach their functional goals? Time for discharge is a debatable topic as we should consider risk for re-injury. Unfortunately, there is little evidence that has determined true mobility and strength requirements to prevent risk of re-injury. Looking at current pain science research, imaging has shown many degenerative changes not being correlated with pain. Because of this lack of correlation, should we even be concerned about mobility and strength impairments at discharge? Some recommend we should use joint and muscle "norms" for determining when our patients should be discharged. Personally, I recommend a standardized mobility evaluation like the Selective Functional Movement Assessment (SFMA) as it improves consistency of examination. However, with aging we can expect some loss of mobility in all planes (not as much as is often assumed). This can make sticking to the norms for discharge difficult. What is recommended is to compare a joint's directional loss to the other directions in the same joint and the same direction in the contralateral joint. This can give you a better picture of what is "normal" for that individual patient. Recently, I had an injury that brought this consideration to mind. As many of our followers know, I have posted several self-management cases about myself. What is interesting is that the majority of the injuries have been on the L side and many of them have been linked to dysfunctional sideglides loading the L side. I recently posted a case discussion video on the Insider Access Page about my recent injury. A couple weeks ago I developed L foot pain that I originally figured was metatarsalgia, however, I later believed it was a neuroma (if looking at it pathoanatomically). The pain was located under MTP joints 2-3 on L side and only during push off in gait. After trying to treat it a couple days with more local repeated motions, I switched to treating the spine. This was due to my history of dysfunctional sideglides on that side and also because I noticed the pain was worst after sitting for longer periods. Historically, I have had a loss of ankle DF bilaterally but worse on the L side. This may have been why I developed the symptoms in the L foot. With the loss of ankle DF mobility, more strain is put on the surrounding joints. Even though I am now pain-free, I need to continue treating myself to improve my ankle DF mobility in order to decrease my risk of re-injury. While I should work to make my mobility symmetrical, I should continue to work on improving ankle DF mobility bilaterally for myself as I am dysfunctional according to the SFMA. Check out the Insider Access Page for the full video demonstration and discussion on this self-management case. -Chris
0 Comments
Leave a Reply. |
Dr. Brian Schwabe's NEW Book in partner with PaleoHacks!
Learn residency-level content on our
Insider Access pages We value quality PT education & CEU's. Click the MedBridge logo below for TSPT savings!Archives
July 2019
Categories
All
|







 RSS Feed
RSS Feed